Clinical decision-support (CDS) software can help sharply reduce the number of CT studies performed in children to evaluate them for possible appendicitis -- without negatively affecting patient care, according to research published in the May issue of Pediatrics.
A team from Children's Hospitals and Clinics of Minnesota in Minneapolis developed CDS software that provides imaging recommendations based on risk algorithms for pediatric appendicitis. After integration into the institution's electronic health record (EHR) and adoption in clinical practice at two pediatric emergency departments (EDs), the CDS software cut CT utilization by more than half for these patients (Pediatrics, May 2016, Vol. 137:5).
What's more, the benefit came without a statistically significant difference in missed appendicitis or negative appendectomies.
"Risk stratification can help to standardize the care of patients with acute abdominal pain," lead author Dr. Anupam Kharbanda told AuntMinnie.com. "Other hospitals that would like to see long-term change should consider integrating the care pathway and associated risk algorithms into their [electronic health record]."
Standardizing patient care
While CT has been touted as a means for improving diagnostic accuracy in patients with suspected appendicitis, recent increases in CT utilization in the U.S. have failed to meaningfully decrease rates of appendiceal perforation. There's an increasing consensus on the need to limit unnecessary CT scans in this patient group due to the risks of radiation exposure, according to the authors.
Influenced by published reports from other hospitals and reports in the literature on the risks of CT, the hospital sought to reduce reliance on the modality and standardize the care of patients with acute abdominal pain at its two urban tertiary care pediatric emergency departments, Kharbanda said. Because clinicians don't always adhere to care pathways, the group also wanted to leverage its EHR (Cerner) for the project.
"Therefore, we attempted to integrate our appendicitis care pathway and algorithms into the ED clinical workflow," he said.
A multidisciplinary team was formed to develop an evidence-based clinical practice guideline. The team included one pediatric surgeon, three pediatric emergency physicians, one pediatric radiologist, and members of the hospital's information technology (IT) department. The group met over a seven-month period in 2011 and agreed to the guideline as well as the process for integrating it into the clinical workflow.
The internally developed CDS software comprises three components:
- A standardized abdominal pain order set for pain medications and laboratory options
- A web-based stratification tool for classifying patients based on risk categories
- An alert provided at the time of ordering imaging studies
The CDS algorithm recommends surgical consultation before diagnostic imaging in high-risk patients (greater than 90% chance of appendicitis), with imaging then ordered at the surgical attending physician's discretion. On the other hand, it recommends that low-risk patients (less than 5% chance of appendicitis) be discharged without imaging and receive outpatient or ED follow-up in 12 to 24 hours.
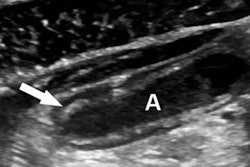
The software recommends a focused abdominal ultrasound study for the remaining patients classified as medium-risk; a surgical attending physician could consider using CT, however, if the ultrasound was equivocal or unavailable or if he or she requested it.
"The risk stratification tool was provided as guidance, to be used in conjunction with clinical judgment," the authors wrote.
When a clinician attempts to order a CT or ultrasound scan to evaluate for suspected appendicitis in pediatric patients, a best-practice alert appears and provides guidance on risk stratifications and recommendations for imaging.
The standardized approach and CDS software were introduced to clinicians in the radiology, surgery, and emergency medicine departments over a four-week period in October 2011, and the new system was launched in early November 2011. The researchers then monitored the performance of the guideline on a monthly basis and provided summary reports to department medical directors after the first year.
Quality improvement study
The researchers also assessed the performance of the project in a three-year quality improvement study involving 2,803 pediatric patients with acute abdominal pain. Of these, 767 were evaluated prior to adoption of the CDS software and 2,036 were assessed after implementation. The patients in each group did not differ significantly in terms of demographics or appendicitis rates.
| Impact of clinical decision support on CT use | ||
| Before CDS | After CDS | |
| CT utilization per patient | 38.8% | 17.7% |
| Ultrasound utilization per patient | 45.7% | 59.7% |
The average 3.5% monthly decrease in CT imaging studies differed significantly (p = 0.007) from the preimplementation period and led to a 54% overall drop in CT utilization by the end of the study. However, ultrasound utilization had already been climbing at a rate of 2.7% each month prior to adoption of the CDS system, and the 1.4% increase after implementation did not reflect a statistically significant change, according to the group. Total imaging utilization (i.e., the percentage of patients who received any type of imaging) also did not differ significantly following implementation of CDS.
Importantly, there were no statistically significant differences between the two study periods for missed appendicitis rates, revisits by patients to the ED within 30 days, appendiceal perforation, or ED length of stay, according to the researchers.
"We have demonstrated that a multicomponent CDS, linked within the EHR, providing guidance for the management of patients with possible appendicitis can reduce the use of CT while maintaining safety and high-quality care for patients," the authors wrote.
For those institutions contemplating a similar CDS initiative for pediatric appendicitis, Kharbanda advised working with a multidisciplinary team that includes representatives from the IT department.
A federally funded project is currently underway to implement the appendicitis care pathway into general emergency departments, he noted. Hospitals in Minnesota and California are participating in the initiative.