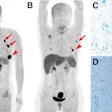
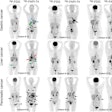
PET with the radiopharmaceutical fluorine-18 fluorodopa (F-18 FDOPA) can help differentiate recurrent or progressive brain metastases from late or delayed radiation injury, according to a study published in the January issue of the Journal of Nuclear Medicine.
Researchers found that F-18 FDOPA PET achieved excellent diagnostic accuracy for patients for whom MRI indicated recurrent or progressive brain metastases. FDOPA-PET was also useful in predicting progression-free survival after radiation treatment.
The study was led by Dr. Karlo Lizarraga from the department of neurology at the University of Miami's Miller School of Medicine (JNM, January 2014, Vol. 55:1, pp. 30-36).
Recurrence versus injury
Patients with cancer that has spread to the brain often receive radiation therapy as part of their treatment. Unfortunately, radiation injury to normal brain tissue can result, making it difficult to distinguish between recurrent or progressive brain metastases (RPBM) and late or delayed radiation injury (LDRI).
It's difficult to noninvasively differentiate recurrence from radiation injury because "both types of lesions can have similar clinical presentations, such as seizures, focal neurologic deficits, and increased intracranial pressure," Lizarraga and colleagues noted. "Second, both types of lesions can have similar MR imaging appearances, such as perilesion edema, rim-like enhancement, and central hypointensity on T2-weighted imaging."
Radiation injury, or necrosis, can occur in 3% to 24% of patients three months to 13 years after radiation therapy, previous studies have found. Treatment options differ for recurrence and radiation injury, so being able to distinguish between the two types of lesions can help physicians choose the most effective therapy path.
PET with FDOPA
There is some precedence for F-18 FDOPA PET's efficacy in this area. A 2006 study found that FDOPA-PET was more accurate than FDG-PET for imaging low-grade tumors and evaluating recurrent tumors in the brain. F-18 FDOPA PET "may prove especially useful ... for distinguishing tumor recurrence from radiation necrosis," the study authors concluded (JNM, June 2006, Vol. 47:6, pp 904-911).
Regarding the current retrospective study, Lizarraga and colleagues believe it's the first "to investigate the diagnostic value of F-18 FDOPA PET for the differentiation of RPBM from LDRI in metastatic brain tumors," they wrote.
Between November 2004 and March 2012, 32 patients (26 women, 6 men; median age, 58 years) with 83 irradiated brain metastases were imaged with F-18 FDOPA PET. They were all referred for the scans after MRI or clinical symptoms suggested they were experiencing recurrent or progressive brain metastases. All patients had undergone radiation therapy prior to the PET scan.
FDOPA-PET was performed on a dedicated system (ECAT HR or HR1, Siemens Healthcare) for 13 patients, while the other 19 patients were imaged with a PET/CT system (Biograph Duo, Siemens). The radiopharmaceutical was injected intravenously at a dose of 1.1 to 6.6 MBq/kg.
Two experienced nuclear medicine physicians blinded to the patients' clinical information interpreted the PET scans, using MR images taken one week before the PET scans as reference.
Patients were monitored at least every three months unless symptoms prompted otherwise. PET findings were validated with a pathologic diagnosis of samples from surgical resection (nine lesions) or radiographic diagnosis (74 lesions) within six months of the PET scan.
For patients who did not undergo surgery, lesions that shrunk or remained stable on contrast-enhanced, T1-weighted MRI after at least six months of follow-up were considered to be the result of radiation injury. Lesions that increased in size by at least 25% were considered recurrences.
Among the 83 lesions included in the study, 32 (39%) were classified as recurrences and 51 (61%) were determined to be radiation injury. FDOPA-PET was able to differentiate between recurrence and radiation injury with a sensitivity of 81%, specificity of 84%, and accuracy of 83%.
Survival rates
FDOPA-PET results also strongly indicated progression-free survival, the researchers found. Lesions with negative FDOPA-PET results had a mean time to progression of 76.5 months, compared with 16.7 months for positive FDOPA-PET results.
The results of the study "demonstrated that F-18 FDOPA PET could distinguish between RPBM and LDRI with a high diagnostic accuracy ... in a population of patients in whom RPBM was suggested by MR imaging," the authors concluded.
Lizarraga and colleagues noted several limitations of the study, including the small number of participants and retrospective approach, which could produce selection bias. In addition, the time between the completion of radiation treatment and PET imaging ranged from four months to nine years.
The current study's findings should be validated in larger prospective studies, they wrote.