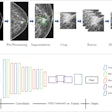
Singh and colleagues trained their prototype machine-learning algorithm to detect and classify chest radiographic findings on 112,000 frontal projection chest x-rays from the U.S. National Institutes of Health (NIH), as well as on 185,000 frontal chest x-rays from the Prostate, Lung, Colorectal, and Ovarian (PLCO) Cancer Screening Trial database.
They then processed 689 anonymous chest x-rays from adult patients and used the machine-learning model to find abnormal masses, nodules, collapsed lung (also known as atelectasis), fluid on the lungs (pleural effusion), enlarged cardiac conditions, and other abnormalities. Two thoracic radiologists assessed all 689 chest x-rays for the presence or absence of these findings.
How well did the machine-learning algorithm perform? The model determined that 51% of the chest x-rays were normal, 25% had one abnormality, and 24% had multiple findings.
The algorithm was most proficient at detecting a collapsed lung (22%), followed by pleural effusion (19%), cardiac abnormality (17%), nodules (15%), and unusual masses (6%).
The machine-learning approach also helped boost sensitivity and specificity for the conditions. Pleural effusion ranked the highest, with sensitivity of 94% and specificity of 93%. Cardiac conditions reached 93% sensitivity and 88% specificity, followed by a collapsed lung, with 83% sensitivity and 73% specificity.
"The machine-learning algorithm accurately detects and classifies chest x-ray abnormalities with higher accuracy for pleural effusion and cardiac silhouette than the pulmonary findings," Singh and colleagues concluded, and could "serve as a second reader for radiologists to improve their accuracy."