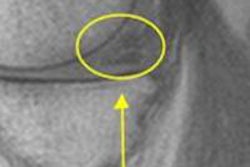
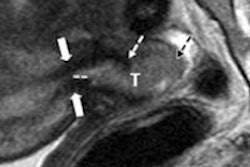
"DWI indirectly provides information on tissue cellular structure and can help in differentiating between hypercellular tissues, such as a tumor, and low or normocellular tissues, such as scar tissue and healthy organs," explained lead author Dr. Doenja Lambregts, PhD, from Maastricht University in the Netherlands.
The study's 117 participants previously had undergone rectal cancer treatment, consisting of standard surgical resection with or without neoadjuvant chemoradiotherapy, a local transanal excision, or a nonoperative "wait-and-see" strategy.
All participants underwent one or more 1.5-tesla MRI scans including DWI as part of routine follow-up or because of a suspected local recurrence after surgery.
Among the 27 patients (23%) with local recurrence, DWI accurately detected the recurrence in 23 (85%).
The other 90 patients with no local recurrence underwent a total of 261 follow-up scans, of which 194 (74%) consistently remained true negative on DWI. Fifty-seven DWI scans could not be adequately assessed due to artifacts, and 14 DWI scans were false positive, primarily at the first follow-up scan after surgery. However, half of the 14 false-positive scans were found to be normal with further follow-up.
The benefit for rectal cancer patients, Lambregts said, is that when they're being monitored after primary treatment, "DWI can help in detecting potential tumor recurrences in an early phase, allowing timely surgical interventions."
The researchers plan to incorporate DWI into their daily clinical practice when following patients after primary rectal cancer treatment. "Furthermore, DWI is part of our follow-up protocol in our ongoing trials where patients are treated with wait-and-see policy or local excision after chemoradiotherapy," Lambregts said.