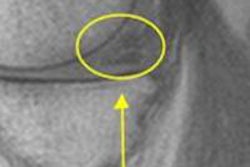
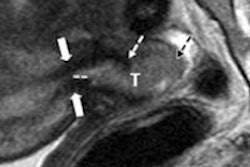
Study results showed that functional MR sequences increased specificity by more than 90%, and dynamic contrast-enhanced (DCE) MRI alone distinguished recurrent sarcoma from postsurgical scarring.
The key is how 3-tesla MRI provides improved signal-to-noise ratio, allowing some of the anatomic sequence parameters to be adjusted for high spatial resolution while maintaining image quality, according to lead author Dr. Laura Fayad, an associate professor of radiology, orthopedic surgery, and oncology at Johns Hopkins.
The study included 58 patients referred for postoperative surveillance with MRI following resection of soft-tissue sarcoma. The goal was to assess the effects of adding dynamic DCE-MRI and quantitative DWI with apparent diffusion coefficient (ADC) maps.
"With these techniques, we will be able to confirm or rule out recurrent disease with greater confidence," added Fayad, who also serves as the director of translational research for diagnostic imaging at Johns Hopkins. "In this way, a patient who has a nodular area of enhancement on conventional sequences that is deemed to be nodular scarring on the functional sequences can be saved from being referred for a biopsy, and instead triaged toward follow-up."
Conversely, she added, a patient with suspicious features can be referred directly to biopsy, even when the nodular area of concern is smaller than 1 cm.
Of the 58 studies, there were eight (14%) histologically proven recurrences. Sensitivity for detecting tumor recurrence was 100% for conventional sequences, 60% with the addition of DCE-MRI, and 100% with the addition of DWI/ADC mapping. Specificity for detecting tumor recurrence was 48% for conventional sequences, 93% with DCE-MRI, and 91% with DWI/ADC mapping.
Because conventional MRI sequences do not offer enough specificity, DCE-MRI and DWI are needed differentiate nodular scars from recurrent tumors, according to Fayad.