Patients with diabetes and/or hypertension are at higher risk of COVID-19 brain complications such as bleeding and stroke, according to research to be delivered at the virtual RSNA 2020 meeting. The findings further illustrate the far-reaching nature of COVID-19 disease.
"COVID-19's effects extend far beyond the chest," said study lead author Dr. Colbey Freeman of Penn Medicine in Philadelphia in a statement released by the RSNA. "While complications in the brain are rare, they are an increasingly reported and potentially devastating consequence of COVID-19 infection."
SARS-CoV-2, the virus that causes COVID-19 disease, first affects patients' respiratory systems, Freeman and colleagues noted. But it has increasingly been shown to affect many other body systems as well, including the brain.
To investigate the incidence of critical findings in COVID-19 patients with additional disease, the team conducted a study that included 81 patients who underwent head CT and/or MRI between January and April of this year, indicated by altered mental state or speech or vision difficulties. Seventy-one patients had head CT scans, one had a brain MRI scan, and seven had both exams. Mean age of the patient cohort was 66.
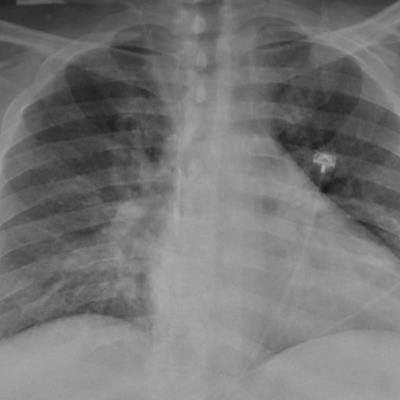
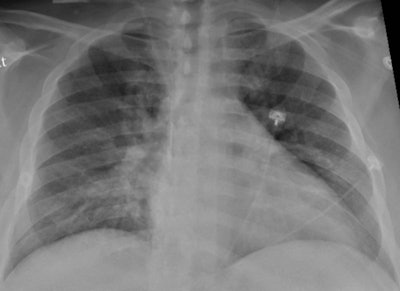 Chest x-ray of a SARS-CoV-2-positive patient exhibiting confusion and showing weakness on his left side shows pneumonia in the lower lungs. Image and caption courtesy of the RSNA.
Chest x-ray of a SARS-CoV-2-positive patient exhibiting confusion and showing weakness on his left side shows pneumonia in the lower lungs. Image and caption courtesy of the RSNA.Of these 81 participants, 18 had findings on brain imaging that were categorized as critical, such as strokes, brain bleeds, blocked vessels, or encephalopathy. Of those with critical imaging findings, 72.2% had high blood pressure and 50% had type 2 diabetes; many had elevated blood markers of inflammation (creatinine, D-dimer, and fibrinogen).
"When your body is in an inflammatory state, it produces all these molecules called cytokines to help recruit the immune system to perform its function," Freeman said. "Unfortunately, if cytokines are overproduced, the immune response actually starts doing damage."
The investigators also found that two-thirds of the 18 patients with critical findings on brain imaging were Black, suggesting a need for careful monitoring for brain complications among this subset of patients.
"COVID-19 is associated with neurologic manifestations, and hypertension and type 2 diabetes mellitus are common in individuals who develop these manifestations," Freeman said in the RSNA statement. "These populations may be at higher risk for neurologic complications and should be monitored closely."
Freeman and colleagues plan to continue their research and will investigate the incidence of neurologic complications in COVID-19 patients who require the use of extracorporeal membrane oxygenation, a pump system that circulates and replenishes oxygen in the blood.
"In addition, we have plans to initiate a larger prospective study evaluating delayed, long-term, and chronic neurologic manifestations that may not be known in this early period in the pandemic," Freeman said.