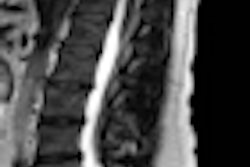
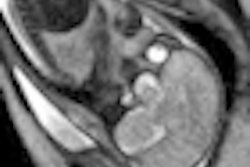
Researchers at the University of Iowa are using proton MR spectroscopy to assess brain abnormalities, shedding light on the development of delirium in bone marrow transplant patients, according to a study presented at this month's RSNA meeting.
Proton spectroscopy shows promise for studying delirium because it measures levels of brain metabolites such as N-acetylaspartate (NAA), choline (Cho), and creatine (Cr), which are essential for cell processes that can offer insight into a disease's physical and biochemical functions.
Previous research has found a high risk of delirium among bone marrow transplant patients and blood stem cell transplant patients. As many as 50% of post-transplant patients experience an onset of delirium within two weeks of transplant.
Despite the high numbers, delirium may go underrecognized and undertreated in nearly two-thirds of cancer cases. "This is often because it is mistaken for anxiety about treatment or treatment side effects," said Jeffrey Yager, PhD candidate, who presented the findings in Chicago. The principal investigator on the study was Leigh Beglinger, PhD, from the University of Iowa in Iowa City.
Negative outcomes
Delirium also is associated with a range of negative outcomes, including increased risk of mortality and longer hospital stay, and is indicative of poor long-term cognitive function. It also can lead to poor communication with physicians and complications with treatments.
"So far, there are very few proton MR spectroscopy studies investigating cognitive function or delirium," Yager added, "but those that do show promise that there may be a brain metabolite imaging biomarker."
In the study, the researchers used proton MR spectroscopy to scan 14 older cancer patients who had undergone a bone marrow transplant. Nine healthy control subjects were also included. Nine bone marrow transplant patients (four males, five females) did not experience delirium, while five bone marrow transplant subjects (four males, one female) were diagnosed with delirium.
All 23 subjects were given a battery of repeatable cognitive tests, once before the transplant day and twice weekly after the transplant. If, after the cognitive tests, the subjects were diagnosed with delirium, they were scanned as soon as possible after onset of the symptoms. At the end of two weeks, subjects who showed no signs of delirium also were scanned.
Delirium demographics
Comparing the three groups showed that the five bone marrow transplant patients with delirium were statistically older (average age of 63.8 years) than the nine subjects with no delirium (average age of 55.4 years) and the nine control subjects (average age of 58.3 years).
The five bone marrow transplant patients with delirium also were statistically more likely to have lymphoma (four cases), compared with the other two subject groups (one total case). However, among the nine bone marrow transplant patients with no delirium, there were four cases of leukemia and four cases of multiple myeloma, compared with no cases of leukemia and one case of multiple myeloma among the five bone marrow transplant patients with delirium.
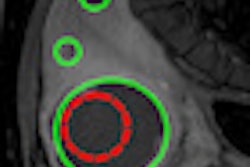
In the researchers' analysis of metabolite activity and peaks, they measured the median of each metabolite. Two different ratios showed significant differences among the three groups.
The NAA/Cho ratio was lower in the bone marrow transplant-delirium group, compared to both the control group (p = 0.012) and the bone marrow transplant-no delirium group (p = 0.037). The Cho/Cr ratio also was higher among bone marrow transplant-delirium subjects than in the bone marrow transplant-no delirium group (p = 0.049).
Subject demographics
|
||||||||||||||||||||||||||||||||||||||||
| BMT = bone marrow transplant. |
Metabolite effects
The elevated choline and reduced NAA levels, Yager and colleagues concluded, could indicate inflammatory processes and white-matter brain damage, as well as neuronal metabolic impairment.
Further research is needed to separate the choline peaks and determine whether a higher choline concentration is a function of the delirium process, or whether it's due to cancer treatment effects, they noted.
As mentioned, the lymphoma diagnosis was associated with delirium. "Further investigation on that treatment would be useful," Yager said, "along with the need for detailed medication logs in future studies."
In addition, the choline peak for proton MR spectroscopy is made up of several different metabolites that can contain choline. While proton MR spectroscopy is unable to distinguish between those metabolites, Yager said that phosphorous MR spectroscopy in combination with proton MR spectroscopy could determine which of those metabolites would be elevated.
The group also recommended that longitudinal studies be conducted to determine if proton MR spectroscopy scans of bone marrow transplant patients may help predict delirium.
By Wayne Forrest
AuntMinnie.com staff writer
December 16, 2010
Related Reading
MRS helps diagnose traumatic brain disorder in athletes, December 2, 2010
MR spectroscopy with MRI detects prostate cancer recurrence, August 4, 2010
MRI/MR spectroscopy falls short for prostate cancer, April 23, 2009
MRS results could steer first-episode psychotics to more aggressive therapy, October 31, 2006
MR spectroscopy aids breast cancer diagnosis, June 8, 2006
Copyright © 2010 AuntMinnie.com