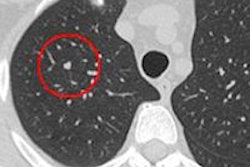
CHICAGO - Reading lung CT scans concurrently with computer-aided detection (CAD) is much faster and about as accurate as first reading the images unaided, and then following up with CAD, concludes a study presented on Wednesday at the 2010 RSNA meeting.
Researchers from Kobe University in Japan said there is no significant benefit to following the traditional reading protocol of unassisted interpretation first, followed by CAD as a second reader.
"While there are many studies showing that radiologists' sensitivity can be improved using second-read CAD, where the radiologist is allowed to view the output of CAD software only after unaided reading, concurrent-read CAD, where the radiologist can view the CAD output without restriction, deserves more attention," said Sumiaki Matsumoto MD, PhD, in his presentation. A previous study by the group found that the main difference in results was the shorter reading time, he added.
Matsumoto and colleagues directly compared concurrent- and second-read CAD on low-dose CT with second-read CAD on standard-dose CT in terms of the observer performance and reading time for lung nodule detection.
The researchers evaluated noncalcified nodules larger than 4 mm in 48 patients, each of whom underwent two CT acquisitions in a single session consisting of a standard-dose (150 mAs) and a low-dose (25 mAs) thin-section CT dataset. Patients consented to the standard-dose scan for evaluation of a suspicious nodule seen at initial low-dose CT, Matsumoto said.
The ground truth status of each of the 187 nodules was determined by two board-certified chest radiologists before the study reading began. For the reading study, four radiologists interpreted each dataset independently using a prototype CAD system (Toshiba Medical Systems, Otawara, Japan) in three sessions at intervals two weeks apart.
At one session for each pair of datasets, each reader interpreted one of the following:
- 25 mAs images with concurrent-read CAD
- 25 mAs images with second-read CAD
- 150 mAs images with second-read CAD
"The order of A-C for the three sessions was systematically varied across pairs," Matsumoto said. Observer performance for each reading session in A, B, and C were mutually compared using jackknife free-response receiver operator characteristics (JAFROC) analysis, and the reading times in A, B, and C were mutually compared using paired t-test for each reader.
The radiologists rated each nodule on a four-point scale, ranging from 0, "definitely not a nodule," to 3, "definitely a nodule," Matsumoto explained.
"JAFROC analysis revealed no significant difference among the three reading paradigms for the four readers" (p > 0.5), he reported. In addition, "when observer performance in A, B, or C was compared with observer performance in the unaided reading part of either B or C, a significant difference was only found between C and the unassisted reading part."
For all readers, while there was no significance difference between the reading times in B and C (p > 0.05), the reading time in A was significantly shorter than that in B or C (p < 0.01).
Observer performance based on figure of merit (FOM)* in radiologists
|
||||||||||||||||||||||||
| *FOM is a modified Wilcoxon statistic indicating that the rating score for a true-positive finding exceeds the rating score for a false-positive finding. FOM ranges from 0 (worst possible reading score) to 1 (best possible score). |
The performance of readers at concurrent- or second-read CAD on low-dose CT was comparable to that of second-read CAD on standard-dose CT, he said. The reading time in concurrent-read CAD on low-dose CT was significantly shorter than that in second-read CAD on low- or standard-dose CT.
"For lung nodule detection, concurrent-read CAD on low-dose CT can allow a similar level of observer performance while significantly reducing reading time as compared to second-read CAD on low-dose or standard-dose CT," Matsumoto concluded.
In response to a question from the audience, Matsumoto said that sensitivity for the investigational CAD system was fairly low at about 60%, with approximately one false-positive per dataset.
By Eric Barnes
Auntminnie.com staff writer
December 2, 2010
Related Reading
Less invasive lung cancer staging strategy has multiple benefits: study, November 24, 2010
Bifurcation filter cuts false positives in lung CAD, October 29, 2010
New CAD for COPD parses disease type, severity, October 1, 2010
Bundling of CAD software boosts lung lesion detection at CT, September 21, 2010
Lung CAD shows promise as concurrent reader, January 30, 2009
Copyright © 2010 AuntMinnie.com