Use of computer-aided detection (CAD) technology helps improve the detection of lung nodules, according to two studies presented at the 2006 RSNA meeting in Chicago.
"For lung cancer screening, (CAD is) a helpful second reader," said Dr. Andre Pereira of Mount Sinai Hospital/University Hospital Network in Toronto.
To evaluate CAD software for nodule detection in a lung cancer screening setting, the researchers performed a retrospective review of 250 low-dose CT scans (1.3 mm, 60 mAs, 120 kV), which were read by two chest radiologists. The studies were then processed and analyzed using ImageChecker CT V2.1 software (R2 Technology, Sunnyvale, CA).
All of the CAD entities were then reassessed by a chest radiologist, and characterized as true positives (a solid nodule found by CAD and confirmed by radiological reassessment) or false positives (any CAD-identified entity that was not a parenchymal nodule).
Nodules found in the double reading but not marked by CAD were regarded as false negatives, Pereira said.
The CAD software placed 1,035 marks, 240 (23%) of which were true positives, according to the researchers. There were 795 false positives, for an average of 3.2 false positives per case.
Of the true positives, 171 were smaller than 5 mm or calcified, and thus regarded as not actionable according to the screening protocol.
The 10 false negatives for CAD included two parenchymal nodules. In addition, eight were surrounded by fibrosis, adjacent to a vessel or a fissure, or were larger than 2 cm, Pereira said. Standalone CAD produced sensitivity of 87% (69 of 79 nodules).
"Technical developments of CAD tools yield a high sensitivity for actionable nodules," he said. "False positives are easily dismissible."
Small nodule detection
In another study, researchers from the University of Rome "La Sapienza" found that CAD improved radiologists' performance in detecting pulmonary nodules on multidetector-row (MDCT) exams.
"The CAD system appears especially useful for the evaluation of small nodules and in particular for less experienced readers," said Dr. Francesco Fraioli. He presented the team's research at the RSNA meeting.
The Italian researchers sought to compare the performance of radiologists against a CAD algorithm for pulmonary nodule detection on MDCT studies, and to evaluate the effect of the CAD system output on the performance of radiologists.
The study team studied 220 asymptomatic subjects with no history of cancer in the previous five years. The patients, who had smoked for at least 15 years, ranged in age from 53 to 64 years old.
Low-dose CT studies were acquired using a Volume Zoom scanner (Siemens Medical Solutions, Erlangen, Germany) using collimation of 4 x 1 mm, 20 mAs, and 120 kV. Scanning time was 22 to 33 seconds.
Three radiologists (with seven years, five years, and one year of experience) independently analyzed each of the studies and assigned a confidence score on a scale of 1 to 3 (1: unlikely; 2: probably; and 3: definitely a nodule). A CAD algorithm was then applied.
Readers then re-evaluated all CAD findings, assigning the same confidence score by consensus. Observers were not allowed to mark any additional nodules or to re-evaluate all of their previous markings, Fraioli said.
For the reference standard, two staff radiologists with 30 and 15 years of experience then reviewed, in consensus, all nodule candidates found by the initial radiologists independently and by CAD. Each true-positive nodule was also classified as peripherally or centrally located, he said.
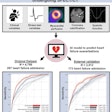
True-positive and false-positive results and confidence levels were then used to generate the free-response receiver operating characteristics (FROC) analysis.
The researchers had sensitivities of 57%, 68%, and 46%, respectively, compared with 92% for CAD. With CAD, sensitivity climbed to 94%, 96%, and 94%, respectively.
The CAD software marked an average of 2.6 false-positive results per each subject (range of 0-7 structures). The researchers found moderate inter-reader agreement, and that the readers required a mean of five, six, and eight minutes, respectively, to interpret each scan. Mean viewing time using the CAD system was seven minutes, according to the researchers.
For all nodules, the area (Az) under the alternative FROC curve was 0.72, 0.82, and 0.55 for the three readers, and 0.84 for the CAD system. The difference between reader 3 and the CAD system was statistically significant, Fraioli said.
For nodules smaller than 6 mm, the Az was 0.40, 0.47, and 0.14, respectively, for the three readers, and 0.72 for the CAD system. The difference in Az between all readers and the CAD system was statistically significant (p < 0.05).
"With the recent introduction of the new class of 64-row CT scanners, CAD systems will have an important role for radiologists to efficiently review and interpret the vast amount of data offered," Fraioli said.
By Erik L. Ridley
AuntMinnie.com staff writer
February 5, 2007
Related Reading
CAD turns in mixed performance for pulmonary embolism, January 16, 2007
Guidelines released for diagnostic testing in suspected pulmonary embolism, December 6, 2006
PET, CT CAD scheme differentiates benign from malignant lung nodules, November 28, 2006
Lung CT CAD boosts performance of less experienced radiologists, November 27, 2006
Barriers still hinder lung CAD adoption, August 24, 2006
Copyright © 2007 AuntMinnie.com