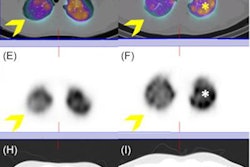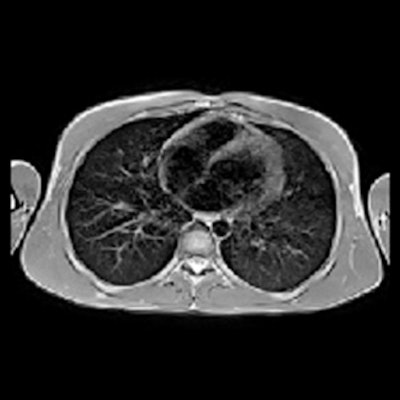
Low-field MRI offers a radiation-free alternative to CT for tracking persistent lung damage in children who have recovered from COVID-19 or have long-haul disease, German researchers have found. Their results were published September 19 in Radiology.
The study underscores the importance of continued monitoring of children who have had COVID-19, even if they appear to have recuperated, noted a team led by Dr. Rafael Heiss of University Hospital Erlangen.
"Our results warrant further surveillance of persistent pulmonary damage in pediatrics and adolescents after SARS-CoV-2 infection," it urged. "Given the already existing diagnostic value of lung MRI and the translatability of the technology, these imaging approaches can be rapidly adopted to clinical routine care."
Some of those who contract COVID-19 experience "long COVID" (defined as symptoms that continue beyond 12 weeks); how long-term COVID manifests in young people has been less clear than how it manifests in adults.
Typically, clinicians use CT to assess COVID-19's effects in adults, but the modality has "limited diagnostic value in children, where lung changes due to COVID-19 are less pronounced," the RSNA said in a statement released with the study. MRI, specifically at low field strengths (0.55-tesla), offers a way to image the lungs that does not require radiation and is able to image alveolar air tissue interfaces, the group explained.
Knieling and colleagues conducted a study that included 54 children (mean age, 11) all of whom were hospitalized with COVID-19 and all of whom underwent low-field MRI after the illness cleared -- although some continued to experience symptoms such as shortness of breath, headache, fatigue, loss of smell, and clouded thinking (29 recovered, 25 with long COVID-19).
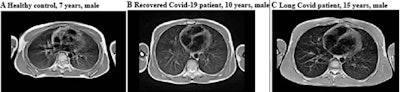 Images acquired in a healthy control (male, 7 years), participant recovered from COVID-19 (male, 10 years) and a participant with long COVID (male, 15 years). Unenhanced axial turbo spin-echo (TSE) sequence with BLADE (periodically rotated overlapping parallel lines with enhanced reconstruction) readout and respiration-gating. Images and caption courtesy of the RSNA.
Images acquired in a healthy control (male, 7 years), participant recovered from COVID-19 (male, 10 years) and a participant with long COVID (male, 15 years). Unenhanced axial turbo spin-echo (TSE) sequence with BLADE (periodically rotated overlapping parallel lines with enhanced reconstruction) readout and respiration-gating. Images and caption courtesy of the RSNA.The primary outcome the researchers assessed was structural changes of the lung parenchyma of the study participants 12 weeks after initial infection compared with MRI information from nine healthy controls who also underwent low-field MRI; the researchers then evaluated lung changes using MRI-derived functional proton ventilation and perfusion parameters (V/Q match), which measures air and blood flow to the lungs, with higher percentages of matching flow indicating better lung health.
Only one of the children who had COVID-19 showed structural changes at the 12-week follow-up MRI exam. But the team did find that the MRI-derived V/Q match percentages were lower among children who recovered from COVID-19 compared with healthy controls.
| MRI-derived V/Q match among healthy, COVID-19 recovered, and long COVID-19 children | |||
| Measure | Healthy control | COVID-19 recovered | Long COVID-19 |
| Ventilation/perfusion match (V/Q) | 81% | 62% | 60% |
The study findings show that lung abnormalities persist among children who have experienced COVID-19 illness -- which is somewhat surprising, Heiss and colleagues wrote.
"As children develop a robust, cross-reactive, and sustained immune response after SARS-CoV-2 infection, the observed pulmonary dysfunction in our study is an unexpected finding," they concluded.