A research team using MRI has found that prenatal maternal distress alters the brain development of their babies, according to a study published April 29 in JAMA Network Open.
The study results highlight the need to support women during pregnancy who are experiencing anxiety, stress, or depression -- not only for their health but for the health of their children, wrote a team led by Yao Wu, PhD, of Children's National Hospital in Washington, DC.
"[Our] findings suggest that altered prenatal brain development in the setting of elevated maternal distress has adverse infant sociocognitive outcomes, and identifying early biomarkers associated with long-term neurodevelopment may assist in early targeted interventions," the authors noted.
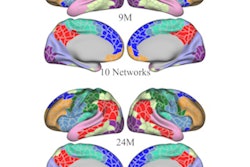
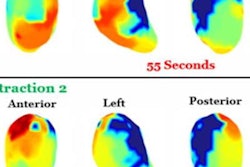
Prenatal maternal distress has been linked to disturbances in fetal brain development, from altered brain volume growth in the amygdala, hippocampal, cerebellar, and cortical gray-matter volumes, to cortical folding, metabolism, and functional connectivity, the group explained.
"Stress-related symptoms are now recognized as the most common complication of pregnancy, affecting approximately one in four women, even those with healthy pregnancies and high socioeconomic status," Wu's team wrote.
But it's not so clear how or if this altered fetal brain development affects children after birth. Using 3D MRI data, Wu and colleagues investigated the neurodevelopment of 18-month-old children who were exposed to maternal psychological stress in utero.
The study included 97 healthy mother-baby pairs. The children had been exposed to maternal distress in utero, which the women had self-reported via a questionnaire. Between 24 and 40 gestational weeks, the mothers underwent 3D, reconstructed T2-weighted MRI exams to assess fetal brain volume and cortical folding. At 18 months after birth, the children's brain development was evaluated using the Bayley Scales of Infant and Toddler Development III and Infant-Toddler Social and Emotional Assessment tool. Maternal stress was also measured at this 18-month juncture with a tool called the Parenting Stress Index-Short Form.
The researchers found that prenatal maternal stress was linked to negative effect on the cognitive performance of their babies (p = 0.01). It was also associated with parenting stress at the 18-month mark after the birth of the babies. Increased fetal cortical local gyrification and sulcal depth were linked to adverse effect on the children's social and emotional performance (p < 0.001 and p = 0.002, respectively) and competence scores at 18-months (p = 0.003 and p < 0.001, respectively).
"We found that increased fetal cortical gyrification index and sulcal depth were associated with decreased infant social-emotional and competence performance," the investigators wrote. "Increased cortical gyrification has been suggested in children with dyslexia and autism, and sulcal depth has been associated with the severity of impaired performance on working memory and executive function in adults with schizophrenia."
The findings are sobering, especially in light of the COVID-19 pandemic, according to the authors.
"More than one million U.S. infants have been born in the COVID-19 pandemic era, yet we lack knowledge about the influence of pandemic-related maternal distress on infants' long-term neurodevelopment," they wrote.
Wu's team's work highlights a need for a holistic care framework during pregnancy, Catherine Monk, PhD, and Dr. Cristina Fernández, both of Columbia University in New York City, noted in an accompanying editorial.
"The findings of Wu et al encourage a whole-person approach to care that monitors and strengthens a pregnant person's mental well-being and quality of life, as well as their physical health," they wrote. "In addition, helping people experiencing distress and other associated factors in the perinatal period could provide support for parent mental health and the brain development of the fetus and future child, thereby presenting a tremendous opportunity for two-generational, public health impact."