PET imaging can predict how liver cancer patients are going to respond early after transarterial radioembolization (TARE), according to a study published online September 8 in the American Journal of Roentgenology.
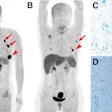
French researchers looked at how patients with hepatocellular carcinoma (HCC) responded to TARE on PET/CT imaging early after treatment using either FDG or an experimental radiotracer called F-18 fluorocholine (FCH). Early PET/CT with either tracer could predict early responses to treatment, as well as patients' overall survival, they found.
"Early posttreatment evaluation with PET/CT could help more reliably identify true nonresponders after TARE, which in turn could prompt early adapted therapeutic management," wrote the group, led by Dr. Edouard Reizine of Henri Mondor University Hospital in Créteil.
HCC is the most common type of liver cancer, occurring most often in people with chronic liver diseases, such as cirrhosis caused by hepatitis B or hepatitis C infection. TARE with yttrium-90 (Y-90), a procedure performed by interventional radiologists, has become widely used in managing HCC. However, imaging criteria to assess whether the treatment is working early on remain a matter of debate.
Treatment response by conventional anatomic imaging -- CT or MRI -- is based on tumor size (modified Response Evaluation Criteria in Solid Tumors [mRECIST]), for instance, and may not become apparent until six months after treatment, according to the authors.
"Consensus is currently lacking regarding the role of early imaging to assess HCC response and predict outcomes after TARE," they wrote.
In this study, the researchers tested whether the early use of PET/CT with FDG or F-18 FCH radiotracers could predict treatment response after six months as well as overall survival rates in HCC patients after TARE.
The retrospective study included 37 patients (34 men and three women) with documented liver cancer treated by TARE at Henri Mondor University Hospital between February 2016 and August 2018. Twenty-eight patients underwent early post-treatment FDG-PET/CT, 15 had early post-treatment F-18 FCH PET/CT, and six underwent PET/CT using both tracers.
Overall patient survival and progression-free survival were assessed based on patient follow-up through June 2019.
Of the 37 patients, 15 (41%) exhibited an early post-treatment PET/CT response based on imaging with at least one of the two tracers, the researchers found. A response at one month (based on mRECIST) was observed in 10 (29%) of 35 patients. Twelve (52%) of 23 patients exhibited an mRECIST response at six months.
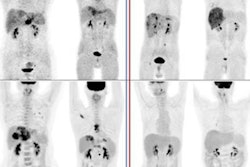
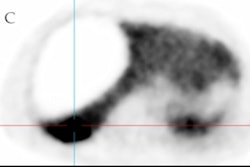
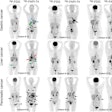
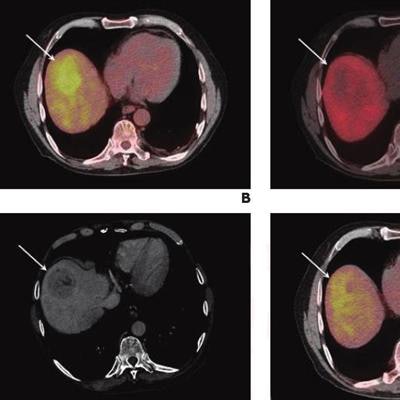
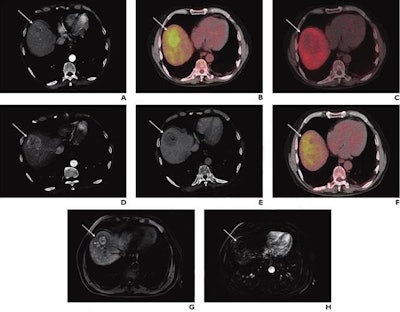 A 74-year-old man with known liver cirrhosis. The patient underwent multiphase contrast-enhanced CT. A lesion in the liver dose (arrow) shows hyperenhancement in the arterial phase (A) and washout in the delayed phase (not shown), consistent with hepatocellular carcinoma. The lesion also shows marked hypermetabolism on FDG-PET/CT (B) but not on F-18 FCH PET/CT (C). The patient underwent multiphase contrast-enhanced CT and FDG-PET/CT one month after radioembolization. The lesion was stable in size and demonstrated persistent hyperenhancement in the arterial phase (D) and washout in the delayed phase (E) but a complete response on FDG-PET/CT (F). The patient underwent MRI six months after the procedure. The lesion shows complete response according to mRECIST, including hyperintensity on unenhanced fat-suppressed T1-weighted imaging (G), without internal enhancement on the subtracted arterial-phase image (H). Image courtesy of the American Journal of Roentgenology.
A 74-year-old man with known liver cirrhosis. The patient underwent multiphase contrast-enhanced CT. A lesion in the liver dose (arrow) shows hyperenhancement in the arterial phase (A) and washout in the delayed phase (not shown), consistent with hepatocellular carcinoma. The lesion also shows marked hypermetabolism on FDG-PET/CT (B) but not on F-18 FCH PET/CT (C). The patient underwent multiphase contrast-enhanced CT and FDG-PET/CT one month after radioembolization. The lesion was stable in size and demonstrated persistent hyperenhancement in the arterial phase (D) and washout in the delayed phase (E) but a complete response on FDG-PET/CT (F). The patient underwent MRI six months after the procedure. The lesion shows complete response according to mRECIST, including hyperintensity on unenhanced fat-suppressed T1-weighted imaging (G), without internal enhancement on the subtracted arterial-phase image (H). Image courtesy of the American Journal of Roentgenology.Early PET/CT response was significantly associated with prolonged overall survival on univariable (hazard ratio = 0.37) and multivariable analyses (hazard ratio = 0.24), the group found.
"Our study suggests that early post-TARE evaluation by PET/CT using FDG or [F-18 FCH] may predict six-month response and [overall survival] in patients with HCC," the authors wrote.
They noted limitations, namely that the study was retrospective and only 37 of 73 patients initially identified were included. Also, because F-18 FCH is experimental, it isn't readily available across practices.
Nonetheless, the key finding of the study is clinically important, they stated.
"Early posttreatment PET/CT could be used to guide early response-adapted treatment decisions," Reizine and colleagues concluded.