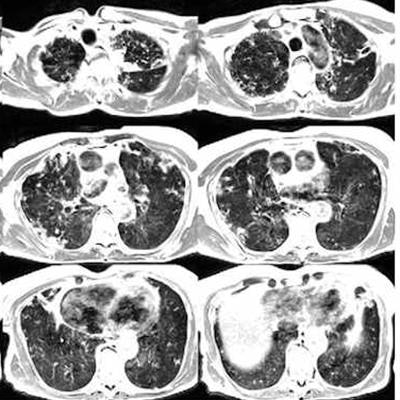
Low-field-strength MRI at 0.55 tesla appears to offer an effective alternative to CT for imaging lung disease, a group of researchers from the U.S. National Institutes of Health has found. The team's study results were published June 10 in Radiology: Cardiothoracic Imaging.
The findings could be good news for patients, since MRI doesn't expose them to radiation, wrote a team led by Adrienne Campbell-Washburn, PhD.
"[MRI] is advantageous over CT because it is free from ionizing radiation, which makes it especially attractive for repeated lung imaging and pediatric imaging," the group noted.
Lung disease is typically evaluated using CT, which produces thin-section volumetric images quickly. MRI offers the benefit of soft-tissue characterization with T1 and T2 image weighting, but since it produces images with lower spatial resolution and takes more time, its clinical role in lung imaging has been restrained, Campbell-Washburn and colleagues wrote.
Yet MRI technology continues to improve. So the researchers sought to investigate whether the use of T1- or T2-weighted lung images, acquired with a low-field strength system, could prove an effective alternative to CT.
The team used a prototype system that consists of a closed-bore 0.55-tesla superconducting magnet that produces "superior field homogeneity compared with contemporary clinical MRI systems (1.5-tesla and 3-tesla) and most implementations of low-field-strength MRI systems," the group wrote.
"At 0.55-tesla, parenchymal T2 is approximately 10 msec, compared with T2 of less than two msec at 1.5-tesla," the authors said. "This improved field homogeneity and prolonged T2 can be exploited to reduce susceptibility artifacts in the lung parenchyma on MR images. In addition, T1 relaxation is shorter at lower field strength ... which is valuable for efficient sequence design."
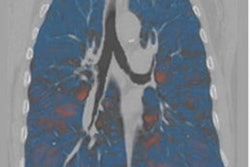
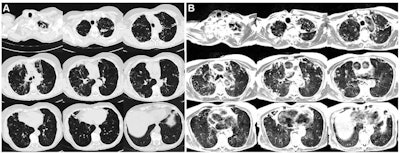 Axial multisection imaging yielded full lung coverage using (A) CT (reformatted to 0.8 x 0.8 x 6 mm) and (B) T2-weighted MRI (1.1 x 1.1 x 6 mm) in a 69-year-old woman with bronchiectasis, cavitary lesions, and scattered pulmonary nodules. Images and caption courtesy of the RSNA.
Axial multisection imaging yielded full lung coverage using (A) CT (reformatted to 0.8 x 0.8 x 6 mm) and (B) T2-weighted MRI (1.1 x 1.1 x 6 mm) in a 69-year-old woman with bronchiectasis, cavitary lesions, and scattered pulmonary nodules. Images and caption courtesy of the RSNA.Campbell-Washburn's team conducted their study between November 2018 and December 2019 and included 24 participants with lung abnormalities; they compared breath-triggered T2-weighted turbo spin-echo MRI at 0.55 tesla with CT scans. The researchers assessed abnormal findings identified with MRI and CT using the kappa coefficient.
The researchers were able to obtain effective lung MR images with an average acquisition time of 11 minutes, and MRI detected a range of lung conditions comparably to CT (measured by kappa coefficient).
| Performance comparison, CT and low-field MRI, in 18 patients | ||
| Imaging finding | Mean kappa value | Percent of scans with 100% agreement between MRI and CT |
| Cavitation | 1 | 83% |
| Consolidation | 1 | 67% |
| Scattered solid nodules | 0.82 | 56% |
| Atelectasis or scarring | 0.56 | 61% |
| Pleural effusion | 0.64 | 83% |
| Bronchiectasis | 0.61 | 67% |
| Ground-glass opacity | 0.57 | 28% |
| Tree-in-bud nodularity | 0.48 | 50% |
Diffuse disease (ground-glass opacities and tree-in-bud nodules) were the hardest to identify on low-field strength MRI, the authors noted.
"This discrepancy might be attributable to the difference in respiratory position between MRI and CT, or it may demonstrate the suboptimal capability of MRI to detect subtle processes causing tree-in-bud and ground-glass opacities," they wrote.
The study results are encouraging, according to the researchers.
"Our findings in this small sample of patients include excellent image quality that shows promise for clinical diagnosis and evaluation of common lung disease," they concluded.