Instructional training increases confidence among family medicine residents using point-of-care ultrasound (POCUS), according to a study published June 4 in Family Medicine.
A team of researchers from the University of New Mexico led by Dr. Jerica Johnson found residents felt "significantly more confident" in their ability to perform and interpret a POCUS exam after a curriculum was implemented and that baseline attitudes toward POCUS were "very" favorable in both the pre- and postintervention surveys.
"Our residents and faculty have all been very excited to use POCUS. There are of course barriers to adoption of any new technology," Johnson told AuntMinnie.com. "The most significant barrier has been residents and faculty feeling that they are trained well enough to use POCUS and that there is not enough time to obtain this training."
The use of POCUS in family medicine residency training is increasing. However, researchers said attitudes about the technology, including confidence levels with performing and interpreting POCUS exams, are unknown.
The team wanted to find out attitudes and confidence levels of family medicine residents before and after the implementation of a new POCUS curriculum.
Residents in their postgraduate years at the University of New Mexico Family Medicine Residency Program were trained with POCUS in a yearlong program. The university's current POCUS curriculum was implemented in 2017.
"We had a loose curriculum with limited POCUS experiences prior to this when we made intentional changes to create a robust POCUS curriculum," Johnson said.
Attitudes and confidence levels with various POCUS exams were assessed through pre and postintervention surveys. On a 5-point confidence scale, a score of 1 meant strong disagreement while 5 indicated strong agreement.
The research team held a three-hour, hands-on workshop for residents, an 18-hour workshop for faculty and residents who participated as volunteer models, and 30-minute sessions every other week for residents who were rotating on the program's inpatient service.
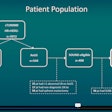
Twenty-one residents responded to the preintervention survey. The average confidence scale score for education on ultrasound principles for performing and interpreting POCUS exams was 4.38. For the postintervention survey, which included 25 residents, that score was 3.96 (p = 0.05).
While agreement was high among residents when it came to ready access to ultrasound equipment and hands-on training, the results did not achieve statistical significance.
The team wrote that future research opportunities include investigating the effectiveness of different POCUS training technologies among family medicine residents and effects on patient-oriented outcomes.
Johnson told AuntMinnie.com that the team is hoping to implement an outpatient-based curriculum for the university's family medicine residents that is geared toward POCUS applications that are useful in the outpatient clinic.
"We are hoping to demonstrate that minimal training interventions can lead to improved revenue generation from the POCUS exams and essentially provide evidence that POCUS training for family medicine residents 'pays for itself,'" she said. "We hope that this outpatient-based curriculum can then be shared and applied by other family medicine residency programs."