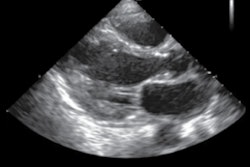
Patients with COVID-19 can experience cardiac injury and dysfunction that can be visualized on echocardiography scans, according to a pair of letters in the Journal of the American Society of Echocardiography. The letters support the idea that echocardiography may provide a noninvasive method to study COVID-19 heart complications.
The presence of left ventricular dysfunction was an important finding in cases profiled by both letters, which were written by teams who used echocardiography on hospitalized COVID-19 patients in Boston and New York City. While the findings described in the letter are preliminary, they provide more evidence that severe cases of COVID-19 can involve cardiac abnormalities.
"Echocardiography remains an essential diagnostic tool in this climate, particularly with emerging data that myocardial injury appears to be associated with adverse prognosis and that echocardiography may add important prognostic information," wrote the group led by Dr. Timothy Churchill of the echocardiography laboratory at Massachusetts General Hospital in Boston.
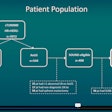
In a study published on May 27, Churchill and colleagues performed 125 echocardiograms requested by physicians on patients with COVID-19. More than two-thirds of patients (69%) were in the intensive care unit (ICU), and the vast majority of these patients required mechanical ventilation and vasopressor support.
More than one-quarter of patients in the study exhibited left ventricular dysfunction, including 22% of patients with impaired left ventricular ejection fraction and 14% of patients showing wall motion abnormalities.
However, left ventricular dysfunction also appeared to resolve for many patients as their COVID-19 symptoms improved. When the authors performed follow-up echocardiograms on 11 patients, 88% showed resolved abnormalities without procedural intervention. Only two patients showed persistent left ventricular dysfunction, and one of those patients had preexisting left ventricular dysfunction.
"Prospective studies, and correlation of echocardiographic data with disease severity, biomarkers, and clinical outcomes, will be required to understand the range of cardiovascular involvement in COVID-19," the authors concluded.
A second letter published on June 5 studied myocardial injury in 110 patients hospitalized consecutively with COVID-19 at Mount Sinai Icahn School of Medicine in New York City. The authors, led by Dr. Karan Sud, used portable ultrasound machines, with scans interpreted by board-certified echocardiography attending physicians.
A total of 37% of hospitalized patients with COVID-19 had isolated left ventricular dysfunction, the team found. Another 17% of patients had right ventricular dysfunction, and 17% had biventricular dysfunction. Only 29% of patients had preserved biventricular function.
Significant myocardial injury was present in 24 patients, the authors noted. A little more than 40% of patients with myocardial injury required mechanical ventilation at the time of the ultrasound scan.
Out of the patients with myocardial injury, 54% had left ventricular dysfunction, and 46% had regional wall motion abnormalities. Another one-third of these patients also had the presence of more than trivial pericardial effusion.
"Regional LV dysfunction appears to be the most common echocardiographic finding, which suggests that ischemia due to large or small vessel obstruction and prothrombotic state may be a common mechanism of injury," Sud and colleagues concluded.
It is important to note that both letters described small, isolated studies on a select population of patients with COVID-19. Nevertheless, they demonstrate cardiac findings, particularly left ventricular dysfunction, may not be uncommon in hospitalized patients with the novel coronavirus.