Chest CT helps clinicians quickly assess the disease severity of patients suspected of COVID-19 pneumonia, as CT findings in patients with severe illness differ from those in patients with milder disease, according to a study published April 11 in European Radiology.
The study results could help physicians better assess patients on presentation, wrote a team led by Dr. Rui Zhang of Renmin Hospital of Wuhan University, Wuhan, China.
"Quick recognition of the radiological manifestations and a prompt evaluation of the patient's exposure history is imperative in early detection and assessment of the severity of SARS-CoV-2 pneumonia," the team wrote.
The SARS-CoV-2 virus appears to have a relatively long incubation time, and individuals often have mild or no symptoms -- which allows the virus to be spread easily, the group noted. The researchers sought to assess whether COVID-19 pneumonia features on chest CT could help determine disease severity.
Zhang and colleagues compared the CT features of 120 confirmed SARS-CoV-2 pneumonia patients. Cases were categorized as "common" versus severe, symptomatic versus asymptomatic, and febrile versus afebrile. Severe cases were categorized as such when a patient had at least one of the following: respiratory distress, blood oxygen saturation of ≤ 93% at rest, oxygenation index of ≤ 300 mmHg, the need for mechanical ventilation, shock, and/or intensive care unit monitoring and treatment.
All patients underwent chest CT on admission. COVID-19 was confirmed with reverse transcription polymerase chain reaction tests. The team assessed lung lobe involvement on a scale of 0 (mild) to 4 (critical) and assigned a total severity score by adding the scores of all five lung lobes (range, 0 to 20).
Of the 120 patients, 16 were asymptomatic, 74 had mild cases, and 30 had severe disease. Of those with severe disease, all were 20 years older on average than those patients with mild disease. Patients with severe disease were more likely to have comorbidities than those with mild disease (73% compared with 11%).
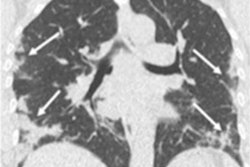
The most frequent CT finding among all patients was ground-glass opacities. Patients with severe disease were more likely to have linear densities, consolidation, "crazy-paving" pattern, white lung appearance, air bronchograms, and pleural effusion.
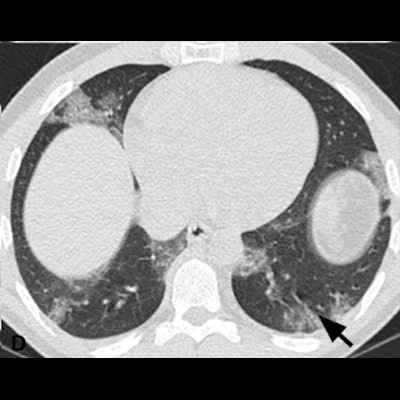
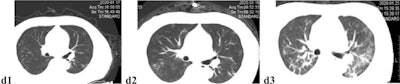 Unenhanced axial CT images of a 52-year-old male doctor with asthma and exposure to patients with confirmed SARS-CoV-2 infection, initially presenting with fever, nonproductive cough, dyspnea, and myalgia, who rapidly progressed to a severe form requiring mechanical ventilation. (D1) Multifocal, limited ground-glass opacity in the periphery of both lungs, predominantly affecting left lung. (D2) Two days later, focal ground-glass opacity has increased in size and density, and new diffuse ill-defined ground-glass opacity has developed. (D3) After four days of mask oxygen supplementation, disease progressed further, with more patchy consolidations and linear densities observed in nearly all lung zones except the anterior part of both lungs. Images courtesy of European Radiology.
Unenhanced axial CT images of a 52-year-old male doctor with asthma and exposure to patients with confirmed SARS-CoV-2 infection, initially presenting with fever, nonproductive cough, dyspnea, and myalgia, who rapidly progressed to a severe form requiring mechanical ventilation. (D1) Multifocal, limited ground-glass opacity in the periphery of both lungs, predominantly affecting left lung. (D2) Two days later, focal ground-glass opacity has increased in size and density, and new diffuse ill-defined ground-glass opacity has developed. (D3) After four days of mask oxygen supplementation, disease progressed further, with more patchy consolidations and linear densities observed in nearly all lung zones except the anterior part of both lungs. Images courtesy of European Radiology.| SARS-CoV-2 pneumonia appearance on CT by disease severity | ||
| CT findings | Common disease | Severe disease |
| Ground glass opacities | 87% | 97% |
| Bilateral | 44% | 93% |
| Linear densities | 56% | 83% |
| Consolidation | 41% | 83% |
| Crazy paving | 10% | 70% |
| White lung | 0% | 67% |
| Air bronchograms | 6% | 63% |
| Pleural effusion | 0% | 30% |
Patients with severe disease had more lung lobes involved (80% had five lobes involved, compared with 7% of those with mild disease), and their mean total severity scores were higher (11.6 versus two).
The group hopes the study findings will allow for appropriate evaluation of patients suspected of pneumonia caused by SARS-CoV-2.
"The typical CT features we described and some radiological findings ... together with some clinic-biological characteristics of severity, may help clinicians in assessing the severity of SARS-CoV-2 pneumonia quickly at admission of patients," the researchers concluded.