Using MRI and PET scans and cerebrospinal fluid (CSF) assays, researchers have collected data on a variety of key biomarkers that might explain whether Alzheimer's disease develops differently in Caucasians and African-Americans. So far, the preliminary findings are creating more questions than answers in a study published online January 7 in JAMA Neurology.
While MR and PET images revealed no significant biomarker differences between the races, CSF samples showed significantly lower levels of tau protein, which is associated with the onset of Alzheimer's, in African-Americans than in Caucasians. In addition, older Caucasians who carry the apolipoprotein E (APOE) ε4 allele, a genetic factor for Alzheimer's, have three times the chance of developing Alzheimer's disease, but the gene variant has a much weaker effect in African-Americans.
So, what are researchers to make of these apparently conflicting Alzheimer's marker results?
"On the surface it suggests that what we have been thinking of as an important risk factor for Alzheimer's disease -- APOE4 -- is important for Caucasians but perhaps operates differently in African-Americans," said lead author Dr. John Morris, distinguished professor of neurology at Washington University School of Medicine in St. Louis. "Whether it helps explain the lower concentrations of tau protein or whether it suggests a different mechanism, we don't have an answer for that yet, but obviously this genetic risk factor has different influences between African-Americans and Caucasians."
Research outreach
The primary reason for the uncertain conclusions is the lack of data in minority populations for Alzheimer's and other neurodegenerative diseases.
 Dr. John Morris from Washington University School of Medicine.
Dr. John Morris from Washington University School of Medicine."We've been doing biomarker research into Alzheimer's disease [at Washington University] for more than 15 years, but we have never before asked the question of whether people from different racial or ethnic backgrounds demonstrate the same biomarker profiles," Morris explained to AuntMinnie.com. "Partly the reason we never asked is because we have a relative paucity of people who are not Caucasian; very few African-Americans, even more rarely did we have Hispanics, Asian-Americans. So we simply did not have the numbers of individuals from nonwhite groups to do any meaningful scientific comparisons."
Morris became the principal investigator at the university's Charles F. and Joanne Knight Alzheimer's Disease Research Center (ADRC) in 1997. At the time, approximately 5% of people enrolled in memory and cognitive studies at the center were African-American, even though they accounted for as much as 18% of the population in the greater St. Louis area.
Given that disparity, Morris and fellow researchers launched an initiative to welcome African-Americans into their program. They subsequently gathered enough data to investigate whether their Alzheimer's biomarker profiles differed from those of St. Louis-area Caucasians.
"We asked that question not because we thought there would be racial differences," Morris said. "It was because in our studies we were combining our information from all individuals. We did not anticipate there would be differences [between the two racial groups], but that is what we found."
The longitudinal study enrolled 1,255 participants (mean age, 70.8 ± 9.9 years), 173 of whom were African-American, from January 2004 through December 2015. Among the subjects, 116 (67%) of the 173 African-Americans were cognitively normal, as were 724 (67%) of the 1,082 Caucasians (JAMA Neurology, January 7, 2019).
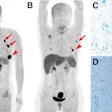
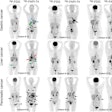
All subjects underwent MRI brain scans, as well as PET imaging with Pittsburgh Compound B (PiB) and/or cerebrospinal fluid assays to determine concentrations of beta-amyloid and tau protein. Analyses were conducted between April 2016 and August 2018 and took into account the subjects' age, gender, educational level, race, APOE ε4 allele status, and cognitive capacity.
Imaging findings
With MRI, the researchers investigated the prevalence or frequency of infarcts in the brains of African-Americans. They also considered whether an elevated risk of Alzheimer's disease might be related to the group's increased tendency for cardiovascular and cerebrovascular risk factors, such as diabetes, obesity, smoking, and high levels of cholesterol. In this part of the study, the researchers found no difference between African-Americans and Caucasians.
Morris and colleagues then used MRI to measure changes in hippocampal volume between the two groups. Alzheimer's disease progresses as hippocampal volume shrinks, adversely affecting memory. Here the researchers found that hippocampal volumes of African-Americans with a first-degree relative with dementia were smaller (6,418.26 ± 138.97 mm3) than those of Caucasians with a family history of dementia (6,990.50 ± 44.10 mm3) -- though the difference was not statistically significant.
However, when there were no family histories of dementia, there were no differences in hippocampal volume. Thus, having a family history of dementia appears to be related to hippocampal volume.
"We found a difference, but again it is puzzling," Morris said. "That is something that we cannot explain, and it deserves a more careful evaluation with a much larger number of African-Americans to tease this apart."
With PiB-PET imaging, the researchers observed similarly increasing amounts of amyloid as Caucasians and African-Americans aged; older adults had a much higher amyloid burden than younger individuals. There were no differences between the races for this biomarker.
As for mean CSF concentrations of total tau, levels were lower on a statistically significant basis in African-Americans (293.65 ± 34.61 pg/mL) than in Caucasians (443.28 ± 18.20 pg/mL) (p < 0.001). The researchers suggested the disparity was due to the degree of APOE ε4 presence in the two groups.
"With tau, the pattern was the same in African-Americans and Caucasians, but the absolute amounts were consistently lower in African-Americans," Morris said. "What this may indicate is that the cutoffs between normal and high levels of tau that were developed by studying Caucasians are probably not accurate for African-Americans and could cause us to miss signs of disease in some people."
What's next?
The researchers hope these findings will underscore the importance of making Alzheimer's disease research applicable to all people, rather than focusing on one ethic group or race. The broader data will provide a better understanding of the illness and potentially lead to more effective treatments, Morris said.
"If we don't open up this research to all racial and ethnic groups, we won't know if what we learned in Caucasians is truly applicable. We need to study the disease in all people," he said. "Not only is this imperative now, but our older adult society -- as is our entire society -- is becoming more and more diverse. So we need to have answers to these very important questions in all groups of people."