Researchers from South Korea used a combination of virtual reality and 3D printing technology to identify and determine the best course of treatment for a lung cancer that was otherwise indiscernible on conventional CT scans, according to a report published online September 25 in Thoracic Cancer.
In the case study, a multidisciplinary team of physicians from Seoul National University Hospital explored management options for a 75-year-old man whose CT exams indicated the presence of inflammation following radiotherapy for a metastatic lung tumor. The patient had a 40-pack-year smoking history and had previously undergone lobectomy for squamous cell carcinoma -- a type of non-small cell lung cancer. A bronchoscopy exam of the inflamed area revealed that the tissue was another recurrent cancer.
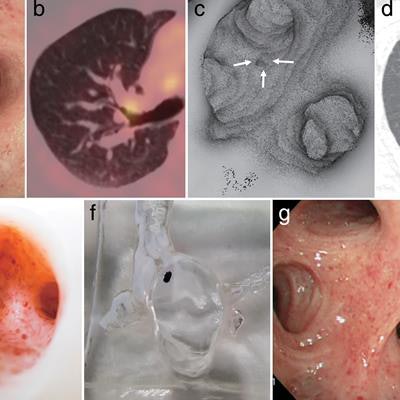
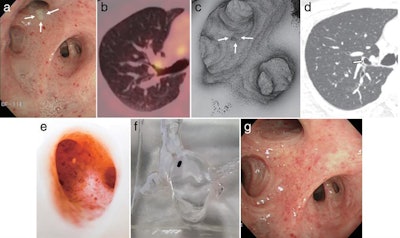 Selection of images from (a) bronchoscopy, (b) PET/CT, (c) virtual reality endoscopy, (d) CT, (e, f) 3D-printed models, and (g) bronchoscopy two months after treatment. Image courtesy of Yoon et al.
Selection of images from (a) bronchoscopy, (b) PET/CT, (c) virtual reality endoscopy, (d) CT, (e, f) 3D-printed models, and (g) bronchoscopy two months after treatment. Image courtesy of Yoon et al.The physicians first attempted to find the exact location of the tumor by acquiring contrast-enhanced CT scans. They found no gross abnormality upon meticulous review. Subsequently, they acquired PET/CT scans and identified a lesion in the right upper lobe of the patient's lung. However, this finding was skewed by misregistration between the PET and CT scans and did not indicate the actual location of the cancer.
"Our case could not be visualized on modern multidetector contrast-enhanced thin-section CT images and was misregistered on fused PET/CT images," first author Dr. Soon Ho Yoon and colleagues wrote. "The multidisciplinary team had difficulty assessing the technical feasibility of the potential treatment options ... as the precise location of lung cancer on the cross-sectional imaging modalities was unknown."
Venturing into more advanced visualization technology to pinpoint the tumor location, the researchers used 3D imaging software (Medip, Medical IP) to reconstruct the CT scans into 3D images for viewing in a virtual reality headset (Vive, HTC). They finally found the tumor lodged within the lung airway by examining the images in virtual reality.
Yoon and colleagues decided to create a 3D-printed model of the airway based on the patient's CT scans to help the physicians determine the ideal treatment strategy. They printed the airway model using a 3D printer (Replicator 2X, MakerBot) and color coded the anatomical structures.
The 3D-printed airway model allowed the clinicians to observe the precise location and shape of the tumor in relation to the complex airway anatomy surrounding it, after which they were convinced that the safest way to treat the patient would be photodynamic therapy. The patient demonstrated no complications on follow-up bronchoscopy two months after treatment
"New imaging techniques including advanced [virtual reality] images and 3D printing enhanced multidisciplinary discussion to make the optimal treatment decision for early lung cancer that was difficult to locate because of radiological invisibility on conventional cross-sectional imaging modalities," they wrote.