An artificial intelligence (AI) algorithm can be highly sensitive for detecting pneumothorax on chest CT images, potentially enabling radiologists to quickly prioritize these life-threatening cases for priority review, according to research from Massachusetts General Hospital (MGH) and Harvard Medical School.
A team led by Xiang Li, PhD, a research fellow at MGH, developed a deep-learning algorithm designed to provide "surveillance" for the presence of pneumothorax on new chest CT studies. In testing, the system yielded 100% sensitivity and more than 88% specificity.
"Use of surveillance programs will allow radiologists to work smarter and sift through their case queues to find the most important results faster, [providing] better patient care, better outcomes, better [public relations] with referring physicians, and better quality of work life for radiologists and referring physicians," said co-author Dr. James Thrall, chairman emeritus of the department of radiology at MGH.
It's also another example of how AI and deep learning will make radiologists better -- not replace them, Thrall said. The researchers presented their findings at the recent American Roentgen Ray Society (ARRS) meeting in Washington, DC.
A life-threatening condition
Pneumothorax is among the conditions detectable by imaging that can be immediately life-threatening, Thrall said.
"Finding one of these is considered a level 1 result and requires live communication between the radiologist and referring physician in our institution within one hour," he said. "Other examples [of a level 1 result] are stroke, heart attack, free air in the abdomen, ectopic pregnancy, spinal cord compression, and bowel obstruction."
Even a small pneumothorax can expose patients to danger during plane travel; as cabin pressure drops, air can expand in volume. Furthermore, pneumothorax is often unsuspected and can occur without classic signs or symptoms, according to the researchers.
As a result, the researchers wanted to develop a surveillance program that could be run immediately after each chest CT scan is completed and would reorder the radiologist worklist to enable the early review of cases likely to be harboring a pneumothorax, he said.
"We envision a suite of such surveillance programs for the conditions like those listed above that radiologists can use to basically give priority to the most serious cases," Thrall told AuntMinnie.com. "This will not only be good for better patient care but will also improve the quality of work life for the radiologist because they will not have to worry about a life-threatening condition on a scan waiting unread on a long work queue."
Deep learning
To assemble training data for their deep-learning model, the researchers selected cases of pneumothorax from the institution's RIS and PACS software using keyword searches for "pneumothorax" and "chest CT." Pneumothorax lesion regions were then manually annotated for each case under the supervision of three senior radiologists.
The researchers used transaxial 3D DICOM images from 341 chest CT scans, including 172 with known pneumothorax and 169 without pneumothorax. They trained a 2D convolutional neural network (CNN) on 50 cases with pneumothorax and 30 cases without pneumothorax; the test set consisted of the remaining 122 cases with pneumothorax and 139 cases without the condition.
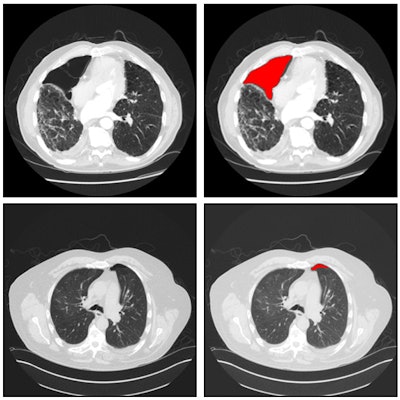
After classifying patches of the images based on their probability of pneumothorax, the seven-layer CNN generates "heat maps" on the images to display the size of the pneumothorax area, the relative location of the region to the lung boundary, and a shape descriptor. A support vector machine classifier was then trained to use this data to classify the chest CT scans as either positive or negative for pneumothorax.
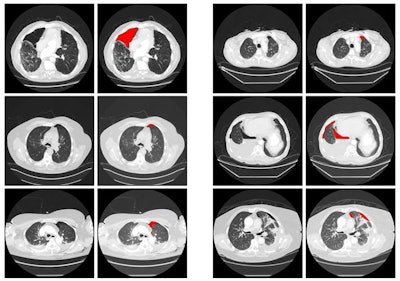 Six example heat maps generated from the patch-wise CNN output, along with input images. Source: Xiang Li, Subba Digumarthy, Mannudeep Kalra, Quanzheng Li, and James Thrall, in research protocol "The application of deep-learning techniques in radiology."
Six example heat maps generated from the patch-wise CNN output, along with input images. Source: Xiang Li, Subba Digumarthy, Mannudeep Kalra, Quanzheng Li, and James Thrall, in research protocol "The application of deep-learning techniques in radiology."In testing, the deep-learning algorithm detected all 122 cases of pneumothorax and had 16 false positives (88.5% specificity). The 16 false-positive results were related to either metal artifacts or bullae associated with chronic obstructive pulmonary disease. However, radiologists can easily recognize these false-positive findings, Thrall said.
Future plans
The researchers are now working to accumulate more cases to further train the model. In light of the false-positive cases in testing, they also plan to add more sample cases with artifacts and lung conditions.
"We are moving to implement this for standard patient care," Thrall said. "That involves many steps and will not happen at MGH overnight."