The growing breadth of clinical applications for interventional radiology is on display at this week's Society of Interventional Radiology (SIR) annual meeting. Talks are running the gamut from artery embolization for knee osteoarthritis to CT-guided cryoablation of nerves that carry hunger signals to assist with weight loss.
Interventional radiologists are developing innovative minimally invasive techniques to treat clinical conditions that are exceedingly common in today's society, according to Dr. Suresh Vedantham, president of SIR and an interventional radiologist with the Washington University School of Medicine in St. Louis. These techniques employ very different mechanisms but are unified by the use of imaging to guide treatment, he said in a press briefing that covered three studies being highlighted at SIR 2018.
"The common theme here really is that it takes the combination of skills in delivering patient care, with a detailed understanding of imaging, and also imaging-guided procedures," Vedantham said. "And really that is the unique skill set that interventional radiologists have that others don't have, and that is our unique contribution to medicine."
Artery embolization for osteoarthritis
Osteoarthritis is an increasingly common problem in the aging population, affecting some 30 million people in the U.S., and it can be frustrating for individuals who want to stay active as they age. The condition typically comes from the deterioration of the lining (synovium) of the knee and manifests as pain, stiffness, and difficulty moving the joints. The most common treatments are short-term, such as joint injections that last only for a few months, or invasive, such as knee surgery, according to Dr. Sandeep Bagla, director of interventional radiology at the Vascular Institute of Virginia.
 Dr. Sandeep Bagla. All images courtesy of SIR.
Dr. Sandeep Bagla. All images courtesy of SIR.Bagla's team has been working with an alternative treatment called geniculate artery embolization (GAE), which involves inserting a catheter through a small incision and guiding the catheter to the genicular artery in the leg. The interventional radiologist then administers small particles through the catheter that block some of the small arteries in the synovium of the knee. This reduces inflammation and pain, Bagla said. The procedure is performed on an outpatient basis.
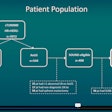
Bagla's group led a clinical trial that is reporting some of the first results with GAE in the U.S. Researchers working at two clinical centers have enrolled 20 patients with severe pain from osteoarthritis, rated as greater than 50 mm out of 100 mm on a visual analog scale. GAE procedures were performed, and patient outcomes were measured and compared with status before treatment; data from 13 of the patients were presented at SIR 2018 on March 19.
All 13 patients successfully completed the procedure; Bagla and colleagues followed up with eight of them one month later. They found that GAE led to a statistically significant reduction in pain (-58 mm, p < 0.016) as reported on the visual analog scale, as well as reduced stiffness and improved physical function. Bagla said the metrics were equivalent to an 80% improvement in function.
He believes that if it's used on a wider basis, geniculate artery embolization could lead to a broad reduction in pain from knee osteoarthritis, possibly also reducing the nation's dependency on opioids as a treatment for pain. Bagla's group hopes to have data from 20 patients by July 2018 and to begin a second study of GAE to determine which patients are the best candidates for the procedure.
T-VEC for liver tumors
In another important talk at SIR 2018, Dr. Steven Raman of the David Geffen School of Medicine at the University of California, Los Angeles (UCLA) discussed a research project he is leading in treating liver tumors through the injection of talimogene laherparepvec (T-VEC), a genetically modified herpes virus being used for oncolytic immunotherapy.
 Dr. Steven Raman.
Dr. Steven Raman.Liver cancer rates have been growing rapidly in the U.S., in large part due to rising obesity rates. While interventional radiology techniques have proved effective for treating early- and intermediate-stage liver tumors, there are fewer options for advanced-stage disease. T-VEC has already been approved to treat melanoma and is now being investigated for liver tumors.
In a study presented on March 21, Raman reported on how researchers from UCLA and other centers investigated the maximum tolerated dose of T-VEC for liver tumors in a phase I safety trial. T-VEC is injected into liver tumors under CT or ultrasound guidance; it then stimulates immunomodulation, in which the patient's own immune system attacks the proteins expressed on the tumor cells.
Raman and other researchers treated 14 patients in the U.S. and Europe with T-VEC, administering the agent every three weeks in escalating doses up to the maximum dose allowed by the U.S. Food and Drug Administration for melanoma treatment. Patients had both primary and metastatic liver cancer. The idea was to find the dose level that was most effective with the fewest side effects, Raman said.
The treatments have been well-tolerated, the researchers found, with the main side effects being flu-like symptoms. The group now plans to move on to a phase II trial to demonstrate the efficacy of T-VEC for this use.
CT-guided cryovagotomy
Also on March 21, Dr. David Prologo from Emory University gave a presentation on the use of CT-guided cryoablation for the treatment of mild to moderate obesity. Obesity has become a major problem in the U.S., with hundreds of millions of dollars spent on weight loss treatments. Despite this, most attempts to lose weight fail.
 Dr. David Prologo.
Dr. David Prologo.Prologo's group wanted to address the phenomenon of diet attrition -- that is, when people abandon their diets, which affects some 95% of dieters. By treating the feelings of hunger that develop when a person is dieting, it might be easier to help individuals stay on a diet and lose weight.
Hunger is actually a signal sent by the body as a survival mechanism when the stomach is empty, telling the person to begin searching for food, Prologo noted. Those signals are carried to the brain by the vagus nerve -- but what if this connection could be short-circuited?
Prologo and colleagues postulated that the same interventional radiology techniques used to freeze the nerves that cause pain could be applied to the vagus nerve in a procedure called CT-guided cryovagotomy. They tested the technique in a group of patients with body mass indexes (BMIs) ranging from 30 through 37 -- above normal but below the threshold for more invasive interventions such as gastric bypass surgery.
At SIR 2018, Prologo presented data from the first 10 patients, who were followed for 90 days. All patients reported a decrease in appetite, and they had an average weight loss of 3.6% of body weight and an average decline of 14% of excess BMI. These numbers are comparable to those from other successful weight loss strategies, he said.
The researchers have now enrolled 20 patients for this pilot study, and next, they want to perform a prospective randomized trial to compare CT-guided cryovagotomy with either standard therapy or a sham therapy as a control.