Smokers have thicker heart walls and less heart-pumping ability on echocardiography scans than individuals who don't smoke, factors that increase the risk of heart failure, according to research published September 13 in Circulation: Cardiovascular Imaging.
What's more, the more years they smoked, the worse heart damage they had, according to a multi-institutional team led by Dr. Wilson Nadruz Jr., PhD, a research fellow at Brigham and Women's Hospital in Boston. Nadruz and colleagues based the findings on data from 4,580 asymptomatic participants in the ongoing Atherosclerosis Risk in Communities (ARIC) epidemiological study who had received echocardiography.
In this elderly population, the researchers found that smoking and cumulative exposure to smoking were associated with higher left-ventricular (LV) mass, a higher LV mass/volume ratio, greater prevalence of LV hypertrophy, and worse diastolic function.
"These findings suggest that active smoking is associated with subtle alterations in LV structure and function, which might help explain the higher risk of heart failure reported for smokers independent of coronary artery disease," the authors wrote (Circ Cardiovasc Imaging, September 13, 2016).
On the bright side, the researchers found that these risk factors appear to be reversible. Former smokers were found to have similar heart structure and function compared with people who have never smoked.
Increased risk for heart failure
While smoking has long been associated with heart attacks and heart failure even in people without cardiovascular disease, no studies to date have discovered a clear mechanism behind this increased risk from tobacco, according to the researchers. As a result, they sought to investigate the relationship between smoking and echocardiography measures in a large cohort of elderly individuals.
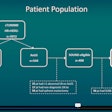
They analyzed 4,580 patients from the fifth visit of the ARIC study who did not have overt coronary artery disease, heart failure, and significant valvular disease, and who had received transthoracic echocardiography. The participants had an average age of 75.7 years and were divided into three categories based on self-reported smoking habits: never smoked (43.2%), former smokers (50.5%), and current smokers (6.3%).
All echocardiography studies were performed by trained sonographers on an iE33 ultrasound scanner (Philips Healthcare); expert technicians analyzed the exams at a central echo core laboratory along with overreading by echocardiographers.
Thicker walls, worse function
After adjusting for potential confounding factors such as age, race, body mass index, blood pressure, diabetes, and alcohol consumption, the researchers found that current smokers had a higher mean left-ventricular mass index, a higher LV mass/volume ratio, and a greater prevalence of LV hypertrophy. They also had worse diastolic function, as measured by the early mitral inflow velocity and mitral annular early diastolic velocity (E/E') ratio.
| Mean echocardiography parameters by smoking history | |||
| Never smoked | Former smokers | Current smokers | |
| LV mass index (g/m2) | 76.7 ± 0.4 | 76.7 ± 0.4 | 80.4 ± 1.1 |
| LV mass/volume ratio (g/mL) | 1.83 ± 0.03 | 1.84 ± 0.01 | 1.93 ± 0.03 |
| Prevalence of LV hypertrophy | 9% | 10% | 15% |
| E/E' ratio | 10.9 ± 0.1 | 11.0 ± 0.1 | 11.7 ± 0.2 |
The differences between those who never smoked and current smokers were statistically significant for LV mass index (p < 0.001), LV mass/volume ratio (p < 0.001), prevalence of LV hypertrophy (p = 0.008), and E/E' ratio (p < 0.001). The differences between current smokers and former smokers were also statistically significant for LV mass index (p < 0.01), LV mass/volume ratio (p < 0.01), prevalence of hypertrophy (p < 0.05), and E/E' ratio (p < 0.01).
"We observed similar echocardiographic features between former and never smokers, suggesting that the potential effects of tobacco on the myocardium might be reversible after smoking cessation," they wrote.
In other findings, the researchers noted that estimated smoking years and estimated pack-years were also associated with greater LV mass index, LV mass/volume ratio, and worse diastolic function (higher E/E' ratio) in current smokers after multivariable analysis.
"The more people smoke, the greater the damage to the heart's structure and function, which reinforces the recommendations stating that smoking is dangerous and should be stopped," Nadruz said in a statement from the American Hospital Association.