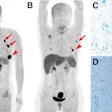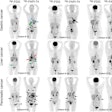
Dual-tracer PET/CT is more effective than contrast-enhanced CT for hepatocellular carcinoma (HCC) staging and may warrant "serious consideration" for use in determining which patients could benefit the most from a liver transplant, according to a study published online January 15 in the Journal of Nuclear Medicine.
PET/CT with a combination of the tracers carbon-11 (C-11) acetate and FDG was significantly less affected by cirrhotic changes, according to the researchers, and it outperformed contrast-enhanced CT in HCC lesion detection and tumor staging among liver transplant patients, as well as in cases of partial hepatectomy.
The lead author of the study was Dr. Tan To Cheung, from the department of surgery at Queen Mary Hospital and the University of Hong Kong.
Milan criteria
The success rate of liver transplants for patients with HCC improves when patient selection is based, in part, on the so-called Milan criteria, Cheung and colleagues wrote. Italian researchers developed the criteria in 1996 to maximize the clinical benefits of liver transplantation.
In their study, Mazzaferro et al found that patients with radiologic evidence of a tumor with a diameter of 5 cm or less, or a maximum of three tumors with a diameter of 3 cm each or less, had an average five-year survival rate of 75% and a disease-free survival rate of 83% (New England Journal of Medicine, March 1996, Vol. 334, pp. 693-699).
While surgical treatment has improved the chances of recovery for HCC patients, the tumor recurrence rate five years after partial hepatectomy can be as high as 80%, according to Cheung and colleagues. In addition, patients with limited liver function are not considered suitable candidates for transplants.
In determining which patients may be best suited for such procedures, CT and MRI have been the modalities of choice. However, the modalities are known to be less effective in detecting HCC in patients with severe cirrhosis, they wrote. More recent studies have found that PET/CT with C-11 acetate and FDG may be more useful in evaluating primary and metastatic HCC disease.
Retrospective review
In the current study, Cheung and colleagues retrospectively reviewed 43 patients (34 men; nine women; median age, 61 years) who had undergone a liver transplant or partial hepatectomy for HCC between March 2004 and March 2010. Among the patients, 22 had liver transplants and 21 had partial hepatectomy. All subjects had also received both preoperative dual-tracer PET/CT and contrast-enhanced CT within a one-month interval.
Under the dual-tracer PET/CT protocol, patients fasted for at least six hours before the injection of C-11 acetate (440-590 MBq). Whole-body imaging was performed from the base of the skull to the upper thigh 20 minutes after injection.
Image acquisition with an integrated PET/CT scanner (Biograph LSO or Biograph 16 LSO Hi-Rez, Siemens Healthcare) began with a no-contrast CT scan, followed by PET. Approximately 15 minutes after completion of C-11 acetate PET imaging, patients received 330 MBq to 520 MBq of FDG. FDG-PET/CT imaging began approximately 60 minutes after FDG administration.
All CT studies were performed with an MDCT scanner (LightSpeed 16, GE Healthcare) and standard contrast-enhanced protocols for dynamic evaluation of the liver. Enhanced images were acquired after intravenous contrast agent injection (Omnipaque 300, GE).
PET/CT images were compared with histopathologic results of explanted and resected livers, as well as other specimens.
Dual-tracer results
Dual-tracer PET/CT performed equally well in the liver transplant and partial hepatectomy groups for the detection of HCC lesions and in tumor-nodal-metastasis (TNM) staging, the researchers found.
Dual-tracer PET/CT detected HCC lesions in 94% of the liver transplant patients and in 96% of the partial hepatectomy group. For TNM staging, it was accurate for 91% of the liver transplant group and 90% of the partial hepatectomy group.
By comparison, contrast-enhanced CT performed "reasonably well" for HCC detection in the liver transplant group (68%), but not as well in the partial hepatectomy group (37%), the authors wrote. In TNM staging, the modality was accurate for 54% of the liver transplant group but only 29% of the partial hepatectomy patients.
The overall sensitivity (97%) and specificity (92%) for dual-tracer PET/CT for patient selection for liver transplantation were significantly greater than those of contrast-enhanced CT, at 42% and 33%, respectively.
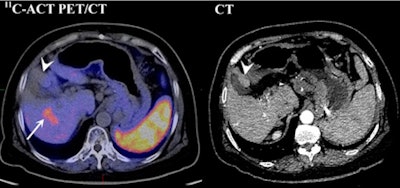 |
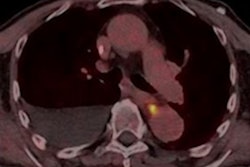
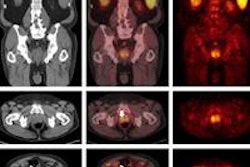
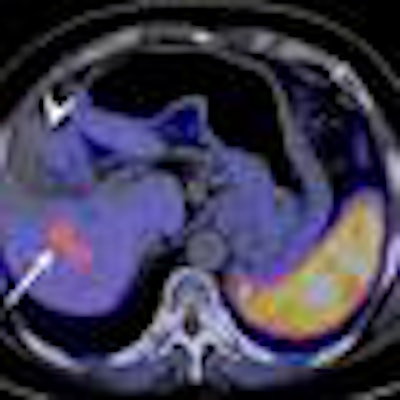
| Contrast-enhanced CT shows nodule impinging on gallbladder, suggesting an HCC (arrowhead) with no abnormal metabolism on C-11 acetate PET/CT. However, a C-11 acetate-avid lesion (arrow) was found. Results of pathological analysis for excised liver confirmed 3.6-cm HCC in right lobe and dysplastic nodule of 2 cm in the left lobe adjacent to the gallbladder. Image courtesy of the Journal of Nuclear Medicine. |
The lower results with contrast-enhanced CT were related to cirrhosis or previous treatment, which can hamper the differentiation of cirrhotic nodules from HCC lesions and the estimation of tumor size, Cheung and colleagues noted.
Transplant selection
Interestingly, C-11 acetate PET/CT was considerably more accurate than contrast-enhanced CT or FDG-PET/CT in determining which patients met the Milan criteria. C-11 acetate PET/CT correctly identified 29 (93%) of 31 patients who met the Milan criteria and correctly excluded 11 (92%) of 12 patients who did not meet the criteria.
FDG-PET/CT alone correctly identified only eight (26%) of the 31 patients who met the Milan criteria and six (50%) of the 12 who did not. Contrast-enhanced CT was correct for 13 (42%) of the 31 patients who met the Milan criteria and for four (33%) of the 12 patients who did not.
"Dual-tracer PET/CT was significantly less affected by cirrhotic changes than [contrast-enhanced CT] for HCC staging and patient selection for [liver transplantation] on the basis of the Milan criteria," Cheung and colleagues concluded.
"The inclusion of dual-tracer PET/CT in pretransplant workup may warrant serious consideration" in determining which patients may benefit most from a liver transplant, they added.