Top Story
Latest News
CT reveals influence of diabetes on COVID-19 severity
April 25, 2024
State of the RT profession more palpable than ever
April 24, 2024
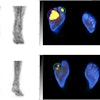
SPECT/CT predicts foot amputations in diabetics
April 24, 2024
Cases of the Week
Check out our Cases of the Week!
More from AuntMinnie
Median posts Q1 results, reports net loss for 2023
April 25, 2024
ScreenPoint CEO steps down; new CEO named
April 25, 2024
Accuray to showcase radiation therapy tech at ESTRO
April 25, 2024
Provisio's SLT IVUS System gets FDA nod
April 25, 2024
Esaote reports growth in fiscal year 2023
April 25, 2024
Next Generation Radiology Workflow Tools
April 24, 2024
Voiant and Thirona enter commercial partnership
April 24, 2024
Spectral AI names CEO of Spectral IP, plans spin-off
April 24, 2024