With more than 5 million Americans afflicted with Alzheimer's disease, the cost of care for people with this most common form of dementia continues to increase.
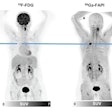
How best to maximize the diagnosis and treatment for patients with Alzheimer's, mild cognitive impairment (MCI), and other forms of dementia could be a function of fluorodeoxyglucose (FDG)-PET.
In its 2007 report, the Alzheimer's Association estimated direct and indirect costs of Alzheimer's and other dementias to be more than $148 billion annually. The amount includes Medicare and Medicaid costs, as well as indirect cost to businesses and their employees who care for persons with Alzheimer's.
The report added that Medicare spent $91 billion in 2005 on beneficiaries with Alzheimer's and other dementias. Those costs are expected to rise to $160 billion by 2010 and $189 billion by 2015.
Past clinical research has analyzed sensitivity, specificity, and accuracy of FDG-PET on MCI and dementia, but few studies, if any, have uncovered FDG-PET's degree of influence on the management of those patients from the referring physician's perspective. With that issue in question, researchers from Kettering Medical Center in Kettering, OH, and Wright State University in Dayton, OH, sought answers.
Discovery dementia
Between March 2004 and August 2005, 96 patients with suspected dementia or mild cognitive impairment were selected for the study, which included 33 females and 63 males with a mean age of 72 years.
Standard questionnaires were sent to 45 referring physicians, requesting details on both pre-PET scan and post-PET scan diagnoses of those 96 patients. The survey specifically asked whether the diagnosis changed based on the PET results.
"This was an important question, because in some patients, we found that the diagnosis changed after the PET scan," said Bhavya Rehani, a research associate at Wright State who presented the study at the 2007 SNM meeting in Washington, DC. "Some new findings came up after the examination, and we wanted to make sure the diagnosis changed based on the PET scan report."
The survey also asked for a list of medications patients were taking -- before and after the PET scans -- and whether medications and treatment management change due to the PET results.
Questionnaires were completed and returned by 41 physicians for a response rate of 76%, or 73 of the 96 patients in the study. Initial surveys were sent three months after the date of the scan, with 51 of the 73 questionnaires returned within six months to one year of the PET procedures.
The researchers found that the FDG-PET information changed the initial diagnosis in 19 of 73 patients (26%) and distinguished Alzheimer's from frontoparietal dementia, striatonigral degeneration, lewy body dementia, Huntington's chorea, and age-related dementia. Because of the FDG-PET scans, the diagnosis changed the disease management in 20 of 73 patients (27%) and prompted the initiation of anti-cholinergic drug therapy in 14 of those 20 patients.
In addition, the PET findings were in agreement with referring physician's initial diagnoses in 53 of 73 patients (73%).
Altering diagnoses
Among the subgroups, the researchers noted that the diagnosis changed from age-related, unspecified memory loss to dementia in five cases. "This was a very interesting subgroup," Rehani added, "because, in these five patients, the physician was not expecting the diagnosis of Alzheimer's disease."
In nine patients, the diagnosis changed from Alzheimer's to age-related memory loss, while the diagnosis on three patients changed from Alzheimer's to dementia.
In all, physicians agreed with the FDG-PET findings in 53 cases, while in 20 patients, physicians disagreed with the FDG-PET results.
FDG-PET brain scanning can be "a powerful tool for the differential diagnosis (26%) and management (27%) of dementia and MCI patients," the researchers concluded, and noted one other finding. "FDG-PET has the potential to increase diagnostic confidence that can confirm the diagnosis, as there is no gold standard" for imaging for Alzheimer's and forms of dementia, Rehani said. PET scan results also provided "better counseling positions to enable caregivers and patients to plan better for the future."
She added that more studies are needed to measure the confidence level, "because we could not quantify the impact of FDG-PET on counseling positions." The report also acknowledged the potential for response bias in the survey results, despite a return rate of 76%, which is comparable to other studies.
By Wayne Forrest
AuntMinnie.com staff writer
September 6, 2007
Related Reading
PET changes oncology management, study shows, July 19, 2007
PET/CT moves closer to diagnostic standard of care, March 1, 2007
Alzheimer's Association funds PET scan study, July 24, 2006
PET more accurate than genetic testing for Alzheimer's, November 10, 2005
PET scan predicts risk of Alzheimer's disease, December 17, 2004
Copyright © 2007 AuntMinnie.com