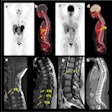
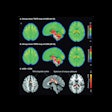
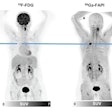
Although FDG-PET is an extremely powerful modality for oncologic staging, its application can be limited by its variable sensitivity and specificity estimates for different metastases in diverse anatomical regions, leading to false negative-findings. Also, inflammation can have a high uptake of the F-18 FDG radiotracer, which can lead to false-positive results.
Over the past few years, a promising technique to increase PET's sensitivity and specificity has evolved: dual-time-point imaging. The protocol of dual-time-point imaging seeks to maximize the uptake of F-18 FDG in malignant tissue, while allowing for the decrease of the radiopharmaceutical in inflammatory tissue. A group of researchers from the Hospital of the University of Pennsylvania (HUP) in Philadelphia recently put this technique to the task of improving breast cancer diagnosis with PET.
"Although PET has been shown to have some potential for breast cancer diagnosis, the variable sensitivities and specificities continue to detract from its diagnostic utility," the researchers wrote (Journal of Nuclear Medicine, November 2005, Vol. 46:11, pp. 1819-1824).
They noted that well-differentiated and lobular carcinomas of the breast have abnormally low FDG uptake that is well below the threshold for its uptake in malignant lesions.
"Consequently, single-time-point SUV analysis is a suboptimal method for assessing suspected breast cancer, and any method to improve the accuracy of PET in breast cancer characterization would be of value in improving the performance of this test," the researchers stated.
The HUP team, which received multinational funding from the U.S. Department of Health and Human Services' National Institutes of Health and the International Union Against Cancer in Geneva, examined 54 women who had 57 breast lesions and were between 32 and 77 years old (mean age 53) in their prospective study.
All the patients underwent multimodality imaging, including MRI, digital mammography, ultrasound, CT, and FDG-PET, the researchers reported. None of the patients had received either chemotherapy or radiation therapy before their PET scans. All patients underwent excision biopsy or mastectomy, with surgical pathology providing the definitive diagnosis against which the PET results were compared.
The PET scans were performed on an Allegro whole-body PET system (Philips Medical Systems, Andover, MA). Two scans were performed on each patient, with an average of 38 minutes between chest-level scans. The first scan was conducted approximately 63 minutes after injection of FDG and covered the whole body from head to toes.
"The second scan included the chest alone, with acquisition of one or two emission scans, resulting in a complete axial length of 25.6 cm to 38.4 cm," the researchers wrote.
Two nuclear medicine physicians analyzed the data independently, and reported identical standardized uptake values (SUVs) in 96% of the cases. A mean was calculated from the two clinicians' observations to derive the final SUV in the remaining 4% of the patients.
After the PET images from the first time point were reconstructed, each physician drew a region of interest (ROI) on four to six PET scan slices at the site of the breast lesion. The slice with the maximum FDG uptake in the ROI was used to determine the SUV. The SUVs for the second time point were obtained with same technique. The study team then calculated the percentage change between the two points.
Of the 57 breast lesions, 39 were determined to be malignant and 18 were determined to be postbiopsy inflammation by surgical pathology.
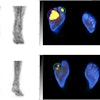
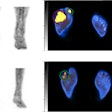
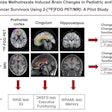
The group reported that there was an increase in FDG uptake over time in the breast malignancies detected with dual-time-point PET and a decrease over time of the FDG uptake in inflammatory lesions and normal breast tissues.
The team observed that the sensitivity of dual-time-point SUV changes was significantly higher than that of conventional single-time-point PET imaging -- 82% compared with 39%, respectively -- in differentiating malignant lesions from inflammatory lesions.
"In the present study, even delayed average SUVs showed a minimal increase in sensitivity from 38% to 41%," the researchers wrote. "Therefore, we believe that changes in dual-time-point SUVs would be a more valuable diagnostic tool than imaging at a delayed single time point alone."
The researchers suggested that future studies extend the time interval between the two scan to 60 minutes to give breast cancer lesions adequate time to accumulate FDG. They noted that this would be feasible for integration into clinical practice, as patients could be staggered between scans.
Although the HUP group called for further research to clarify the benefits of dual-time-point PET imaging in breast cancer, it believes that the increase in diagnostic accuracy through use of the technique more than compensates for the extended length of each scan.
"Dual-time-point analysis is likely to significantly improve both the sensitivity and the specificity of PET in diagnosing breast cancer, as in lung and head and neck malignancies," they wrote.
By Jonathan S. Batchelor
AuntMinnie.com staff writer
December 2, 2005
Related Reading
PEM turns in solid results for detecting breast malignancies, November 10, 2005
PET mammography unit shows promise for DCIS, June 22, 2005
Delayed PET helps delineate gliomas, November 5, 2004
PET sharpens treatment plan for advanced breast cancer, August 16, 2004
PET outperforms CT in breast cancer staging, May 7, 2003
Copyright © 2005 AuntMinnie.com