CHICAGO - Low-dose molecular breast imaging (MBI) can outperform screening mammography to detect cancer in women with dense breasts, according to a study presented on Tuesday at the annual RSNA meeting.
Researchers from the Mayo Clinic in Rochester, MN, used an 8-mCi dose of technetium-99m (Tc-99m) sestamibi rather than 20 mCi in MBI exams on more than 1,600 women with dense breasts. MBI still detected more cancers than mammograms, the group found.
This study is a follow-up to last year's research by lead study author Dr. Deborah Rhodes, associate professor of medicine, and colleagues, who found that adding MBI with 20-mCi Tc-99m sestamibi increased the diagnostic yield for breast cancer from 3.2 per 1,000 for screening mammography alone to 10.7 per 1,000 for the combination of both modalities (Radiology, January 2011, Vol. 258:1, pp. 106-118).
"We have previously demonstrated that the addition of MBI to mammography increased the detection of node-negative breast cancer in dense breasts by 7.5 per 1,000 women screened," Rhodes said.
The study presented at this week's RSNA meeting by Rhodes was performed using two MBI systems composed of detectors from Gamma Medica and GE Healthcare.
All asymptomatic women undergoing routine screening mammography at the Mayo Clinic with heterogeneously or extremely dense breasts on a past mammogram were invited to enroll prior to undergoing either imaging technique.
MBI images were acquired immediately after injection of Tc-99m with two views per breast. Images were interpreted on a five-point scale, following the BI-RADS criteria of 1 as negative and 5 as highly suggestive of malignancy.
MBI final assessment scores of 3, 4, or 5 generated a combined read with a mammogram. Findings not explained by the combined read generated a diagnostic mammogram and ultrasound. If those findings were inclusive, patients received an MRI scan or a six-month follow-up MBI, depending on the level of suspicion.
Currently, there are 1,636 participants in the study (mean age, 58 years). The majority of the women are postmenopausal and have heterogeneously dense breasts.
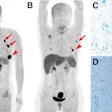
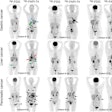
So far, Rhodes noted, 21 women have been diagnosed with cancer. Of those women, the cancer was detected by mammography only in two cases, compared with 14 detected by MBI only. Both modalities discovered the cancer in three cases, and two cancers were missed by both MBI and mammography. In addition, two women had contralateral cancers that were found only by MBI.
Of the cancer detected only on MBI, most occurred in postmenopausal women with heterogeneously dense breasts. "It is interesting to note that three of the participants with cancers detected only on MBI had breasts that were not considered dense," Rhodes added.
In the 14 women with cancer detected by MBI only, 11 cancers were invasive with a median size of 0.9 cm, ranging from 0.5 cm to 4.1 cm. Nine of the 11 cancers were node-negative.
In the four women whose cancers were not detected by MBI, three cancers were invasive with a median size of 0.6 cm, ranging from 0.3 cm to 0.7 cm. All of the cancers were node-negative.
The sensitivity of mammography in this study was 24%, compared with 81% for MBI and 91% for the combination of both modalities. "Because one-quarter of the participants are still awaiting one-year follow-up, we have not yet calculated statistical significance or specificity," Rhodes explained.
The recall rate for MBI (7.7%) was less than for mammography (11%), the group also found.
In addition, while MBI generated 2.2% more biopsies than mammography alone, the positive predictive value (PPV) of those biopsies by MBI was five times greater than that of mammography.
Follow-up results are available for approximately 75% of the study's participants, and "we have demonstrated that we maintained sensitivity for the detection of breast cancer despite substantial lowering of the radiation dose," Rhodes said.
Rhodes and colleagues also compared their results with recently published papers evaluating screening ultrasound and screening MRI for cancer in dense breasts. She said that MBI "compares very favorably to these modalities in terms of the lowest number of images generated per study with the lowest percentage of recalls and highest PPV."
MRI was the only modality with a more favorable diagnostic yield, "but the cost of this modality is a considerable disadvantage in the screening study," Rhodes noted.
She and her colleagues are continuing their research by comparing the incidence and diagnostic performance of MBI using a 4-mCi dose of Tc-99m, which is equivalent to the effective dose of two digital mammograms, she said. A cost efficacy analysis is also under way.
"Important next steps for this technology include multicenter, prospective clinical trials and the direct comparison of MBI to whole-breast screening ultrasound in the dense breast," Rhodes concluded.