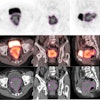
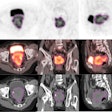
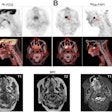
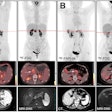
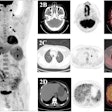
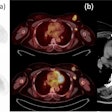
VIENNA - Ever thought of giving your patient an electric shock? The idea may sound like something out of a Frankenstein movie, but more interventional radiologists may soon be doing this if the initial promise of irreversible electroporation, an experimental ablation technique for solid tumors, is supported by further research.
 Prof. Dr. Thomas Helmberger, head of the Institute of Diagnostic and Interventional Radiology and Nuclear Medicine, Klinikum Bogenhausen, Technical University of Munich, Germany. All images provided by ESR.
Prof. Dr. Thomas Helmberger, head of the Institute of Diagnostic and Interventional Radiology and Nuclear Medicine, Klinikum Bogenhausen, Technical University of Munich, Germany. All images provided by ESR."It's very much the new kid on the block," said Prof. Dr. Thomas Helmberger, head of the Institute of Diagnostic and Interventional Radiology and Nuclear Medicine, Klinikum Bogenhausen, Technical University of Munich, Germany. "It has unique features, including preciseness, speed, low collateral damage, and preservation of connective tissue structures."
At yesterday's New Horizons Session, "Ablation beyond radiofrequency," he explained that the technique is based on electropermeabilization, which is a significant increase in the electrical conductivity and permeability of the cell plasma membrane caused by an externally applied electrical field. The method is used in the sterilization and preprocessing of food and is a molecular engineering tool for genes, gene delivery in tissue, transdermal delivery of drugs and genes, fusion of cells, introduction of drugs into cells, and electrochemotherapy for treatment of cancer.
The problem, though, is that reliable information about electroporation is limited, and most studies are only phase II. As of 25 February 2012, there were 159 articles about it on PubMed, only a third of which are clinical. These papers focus on the liver (35), brain (11), kidney (9), lung (6), prostate (5), breast (5), pancreas (3), and bone (3).
"Honestly speaking, there is not much evidence of the technique's use on a large scale," noted Helmberger. "We need more studies on the indications, type of procedure setting -- percutaneous versus open -- optimized protocols, and, most importantly of all, long-term efficacy." Only one device is commercially available at present: the NanoKnife, from AngioDynamics. The number of pulses ranges from 10 to 100, and the pulse length is 20-100 µs ± 2 µs. The maximum current is 50 A, and there are up to six probe channels, he said.
 Prof. José Ignacio Bilbao, professor of radiology at the University of Navarra in Pamplona, Spain, and Congress President of ECR 2013.
Prof. José Ignacio Bilbao, professor of radiology at the University of Navarra in Pamplona, Spain, and Congress President of ECR 2013.The technique leads to the loss of vascular smooth muscle cells. The vessel matrix is not compromised, and it has potential in vascular treatment. Unlike thermal ablation, general anesthesia and cardiac monitoring are essential with electroporation, but there are no immunohistochemical effects, connective tissue is spared, and small vessels are not affected. Only the cell membrane is damaged. Whereas the size of the probe is 14-17G in thermal ablation, it is 16-19G in electroporation, according to Helmberger.
It is important to remember that irreversible electroporation has an electroablative effect and requires a puncture, noted session moderator Prof. José Ignacio Bilbao, professor of radiology at the University of Navarra in Pamplona, Spain, and Congress President of ECR 2013.
Conversely, microwave ablation has a thermal effect and necessitates a puncture, high-intensity focused ultrasound has a thermomechanical effect and needs no puncture, and stereotactic body radiation therapy has an ablative effect and requires no puncture.
Overall, the role of image-guided therapy is to identify the target, to target the target, to select the most appropriate therapy, to monitor the procedure, and to monitor the immediate local effect, he stated.
Percutaneous ablation, either chemical or thermal ablation, is the accepted method of treatment and involves ethanol, radiofrequency, or cryotherapy. The drawbacks are the need for a puncture, unwanted damage to adjacent structures, diminished effects in the vicinity of blood vessels, and ineffectiveness in tumors of less than 3 cm diameter, added Bilbao.
Originally published in ECR Today March 4, 2012.
Copyright © 2012 European Society of Radiology