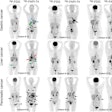
CHICAGO - Researchers at Ohio State University (OSU) Medical Center have found that injection-to-scan time in FDG-PET is "critically important" for accurately and quantitatively evaluating response to therapy, but optimum target times are complicated by patient and technology challenges.
The study, detailed this week at the 2009 annual meeting of RSNA, recommends ways for all institutions to minimize these factors and maintain target injection-to-scan protocols.
"PET quantification is important for diagnosis, response assessment, and accurate reproducible quantifications," said lead author and presenter Dr. Nathan Hall from OSU's department of radiology. "This is especially true in differentiating benign and malignant cutoff with [standard uptake values (SUVs)] and the assessment to the progression of disease and response to therapy."
While there has been "significant criticism" of PET quantification and the use of SUVs, PET quantification is "important, especially if we are going to use PET as a function biomarker," he added.
Target time
The institutional protocol calls for emission scans to begin at 75 minutes after FDG administration, with a range of plus or minus 10 minutes
"At Ohio State University, we went in with the understanding that accurate quantification of response requires a standard injection-to-scan time," Hall said. "Despite the best efforts in maintaining consistent injection-to-scan times, there are multiple factors that impact it, some of which we have little control over and some which we should have better control over."
In reviewing practices at OSU, the researchers found that PET scanners from various vendors can influence optimum patient scan time and SUV results, while scanner software upgrades can produce varying PET quantification results. In addition, a patient's medication or blood glucose level also can affect preferred injection-to-scan times.
The retrospective study included injection-to-scan time for 7,842 FDG-PET studies from 2005 to 2007. The study excluded brain exams due to variable injection-to-scan target times.
The analysis found that OSU's mean injection-to-scan time was 79 minutes, which was within four minutes of the institution's 75-minute target time. Of the 7,842 studies, 5,060 (65%) studies fell within a 65-minute to 85-minute target range, 710 (9%) studies were less than 65 minutes, and 2,117 (27%) studies were above 85 minutes.
Good news, bad news
"The good news is the average injection-to-scan time is within our 75-minute goal," Hall said. "The bad news is that 40% fell outside of the plus or minus 10-minute goal, with a significant percentage (27%) skewered toward longer times."
The primary reason for injection-to-scan times that fell outside of OSU's target time is patient issues. "One of the things that we consistently have a problem with is the patient decides to use the restroom as soon as they are about to go on the scanner," Hall said. "They get lost in there for a significant period of time."
Some patients are positioned in the scanner and "then decide they are claustrophobic," he added. "You need to talk to them to get them back to the scan." Other patients need to be repositioned after moving while on the scanner.
Study recommendations
The researchers concluded that the inconsistencies can make accurate quantification, especially response assessment using SUVs, difficult. "The challenges that we are face are not indicative to only our institution, but are a refection of clinical reality," Hall said.
The study offered several recommendations to optimize injection-to-scan time:
- Schedule clinical trial patients earlier in the day, especially if the clinical trial protocol is different from standard protocols.
- Schedule patients for follow-up scans early in the day to enhance control over consistency assurance with baseline scans.
- Minimize patient factors by giving them adequate time for voiding and dealing with claustrophobia.
- Schedule longer appointment times later in the day to correct for patient motion.
By Wayne Forrest
AuntMinnie.com staff writer
December 3, 2009
Related Reading
Timing is everything in contrast-enhanced CT, September 28, 2006
Copyright © 2009 AuntMinnie.com