CHICAGO - Researchers at Georgetown University Hospital in Washington, DC, have found that radical robotic radiosurgery results in a "distinctive PET/CT imaging pattern" following treatment, which likely is related to high radiation doses delivered 1 cm or more around the tumor.
The study, presented on Sunday at the RSNA annual meeting, followed patients with inoperable stage IA non-small cell lung cancer (NSCLC).
Ten patients had tumors irradiated and then were followed every six months for two years with PET/CT studies. "The tumors that were radiated were small, with an average maximum diameter of 2 cm, but they ranged from 1.4 cm to 3 cm," said Dr. Saloomeh Vahdat, study co-author and presenter at RSNA.
To treat the tumors, three to five gold fiducials were placed under CT guidance 2 cm apart around the tumors. The technique allowed the doctors to irradiate the tumors more precisely "and allowed us to expand the planning target volume by 5 mm," Vahdat added.
Treatment plans
Gross tumor volumes were contoured using lung windows, and margins were expanded by 5 mm to establish the planning treatment volumes. Treatment plans were designed using hundreds of pencil radiation beams, with a mean dosage of 55 Gy (ranging from 45 Gy to 60 Gy) delivered in three equal treatments over a five- to nine-day period.
PET/CT studies were performed (Biograph, Siemens Healthcare, Malvern, PA) with FDG dose between 10 mCi and 15 mCi. "Sixty minutes after FDG injection, low-dose CT and PET images were obtained," Vahdat said. "PET/CT images were corrected for attenuation on the basis of the CT data."
Whole-body FDG PET/CT and contrast-enhanced chest CT scans were performed at six-month intervals following treatment.
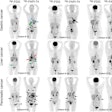
In reviewing average maximum FDG standard uptake value (SUVmax) prior to treatment and then at three- to six-month intervals after radiation, researchers found patterns developing.
Six-month changes
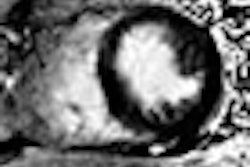
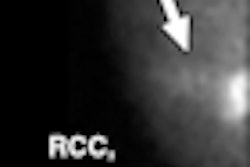
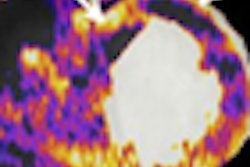
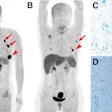
"Typically, at 12 months, we saw an increase in FDG uptake where the radiation took place, which we thought was due to radiation pneumonitis," Vahdat said. "Fortunately, at 18 months, our typical PET/CT scans showed a decrease in FDG uptake where the tumor was treated, which we thought was due to radiation fibrosis."
Prior to treatment, the average SUVmax was 6.2, with a range between 2.2 and 10.9. Three to six months after treatment, the average SUVmax decreased to 2.2, with a range of 1.5 to 4.6. Conversely, at 12 months, the mean SUVmax increased to 3.3 (range, 1.5-5.0) and involved a large peritumoral area, which correlated with radiation pneumonitis seen on CT.
Vahdat said the researchers were surprised to see the increase in average SUVmax at the 12-month mark, "which was probably due to radiation pneumonitis. At 18 to 24 months, we had a decrease in average SUVmax, which was 2.2 again."
There were no local failures or regional lymph node recurrences at a median follow-up of 24 months, she added.
As the researchers concluded that radical robotic radiosurgery to eradicate both gross and peritumoral microscopic disease produces a distinctive PET/CT imaging pattern following treatment, they also recommended additional research to confirm pathologically the PET/CT findings.
By Wayne Forrest
AuntMinnie.com staff writer
November 30, 2008
Related Reading
Chest wall toxicity reported after high-dose lung SBRT, November 26, 2008
Combining chemo and radiation improves NSCLC outcomes for elderly, April 16, 2008
PET/CT beats 3T MRI in whole-body primary tumor staging, March 10, 2008
FDG-PET/CT aids in radiation therapy planning, March 5, 2008
PET does not predict survival in advanced lung cancer, November 29, 2007
Copyright © 2008 AuntMinnie.com